Can you diagnose and tell me what stage of Lipedema I have over Zoom?
No, the diagnosis of lipedema or lipoedema cannot be determined without a physical exam. It is essential for competing for diagnoses to be ruled out and diagnostic clinical signs need to be palpated to make a proper diagnosis of lipedema. Likewise, the stage of lipoedema/lipedema cannot be determined without a physical exam. A physician experienced with lipedema diagnosis will detect nodularity in the skin and subcutaneous tissue and the presence of edema/lymphedema. These factors, plus lobules or festoon/dewlaps.
Is there a blood test to confirm you have lipedema?
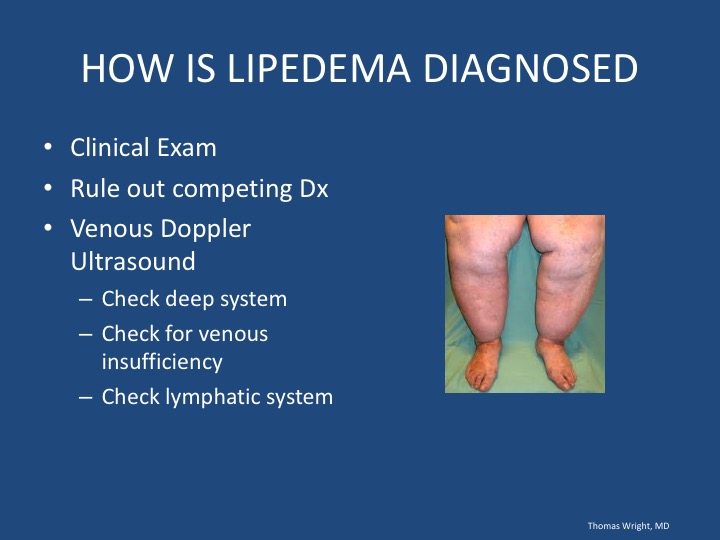
How is lipedema diagnosed?
Many patients are surprised at how thorough the in-office diagnosis and evaluation is – you should expect to spend several hours in the office. We provide in-depth evaluations, including an ultrasound of the affected areas, measurements, full-body photos, questionnaires for symptoms, and in-depth consultation to determine the best treatment options. None of these can be appropriately or adequately provided via web meeting, and we wouldn’t be providing the standard of care we guarantee if we did so.

Will Lipedema have any other health implications or put me at greater risk of other conditions?
The most common complications or health implications caused by lipedema are mobility limitations. Accelerated arthritis of knee and ankles, gait limitation from a bulk excess of adipose around the joints primarily of the knees and ankles. Secondary obesity is partially related to mobility impairments.
Vascular risks are Increased risk of varicose veins and secondary lymphedema, and there can be an increased risk of blood clots associated with lipedema when combined with obesity. Lipedema can cause a small vein vasculopathy that leads to an increase in easy bruising, spider veins [telangiectasias], and varicose veins. If secondary obesity occurs with lipedema, there is an increased risk of DVT or blood clots.
What lipedema treatment options do I have?
Medical or nonsurgical management of lipedema consists of treating secondary lymphedema, if it is present, diet, medications, supplements, and lifestyle changes. Most women with lipedema have secondary edema/lymphedema in their legs and arms. The management of secondary lymphedema focuses on compression garment use, manual lymphatic massage, and pneumatic compression pumps.
Studies have shown that women with lipedema are very insulin sensitive, so we recommend a low carbohydrate diet emphasizing whole food with a low glycemic index. Diosmin which is a supplement extract of citrus fruit, guaifenesin, and amphetamines, have been recommended for the treatment of lipedema. Maintaining an active lifestyle with cardiovascular and resistance exercises is strongly recommended. Water-based exercises can be particularly helpful because they give resistance, cardiovascular, and support lymphatic flow.
What are the risks/benefits of surgery over medical treatment for lipedema?
The likely benefits of lymph-sparing liposuction are decreased pain, heaviness, tenderness, and swelling, and improved mobility, stance, and leg alignment. The potential risks of the surgery are rare but include decreasing the likelihood of lymphatic and skin injury and/or scarring. Risks that are less than one in ten thousand include Blood loss, Deep Vein Thrombosis [Blood Clot], complications from anesthesia, infection, and the least likely complication would be death.
Surgical Considerations for Patient Safety
Patients with Lipedema often have other medical conditions that put them at higher risk for complications. Therefore, all efforts must be made to minimize the risk.
- Lymph-sparing liposuction with a generous tumescent technique that avoids general anesthesia.
- Generally, not more than 5%-8% of the total body surface area should be treated in one surgical procedure.
- Small liposuction cannulas should be used.
- Surgical technique is very important. Intimate knowledge of the locations and anatomic variations of the lymphatic drainage in the limb or body area that is being treated is crucial.
- Patients with significant underlying venous reflux should be treated before having lymph-sparing liposuction.
How long would I likely be bandaged for post-surgery, and how long would I need to wear compression stockings?
Compression after surgery is generally recommended for 2 months. The compression garment is best combined with compression stocking for optimal lymphatic flow and prevention of blood clots. Compression may be required lifelong if there is secondary lymphedema, and the longer patients continue compression therapy, the better outcomes they will have!
How will the Lipoedema/lipedema progress as I get older?
The progression of lipedema is variable. Some women have little or no progression. Other women progress more rapidly. Rapid progression is associated with hormonal and stressful events such as childbirth, menopause, weight gain, and rarely other illness.
Will my insurance cover lipedema surgery?
The general rule of thumb for Lipedema Insurance Coverage claims reimbursements is that any given claim must be deemed “medically necessary.” Lymph Sparing Liposuction is nearly always considered a cosmetic surgical procedure in nature or experimental, meaning this is an elective procedure and not a medical necessity. Of course, as explained above, this is not the case for women with Lipedema, as lymph-sparing liposuction is the only treatment option for dealing with this disease that can reverse progression. However, the combination of the surgery being deemed cosmetic and election plus the general under-education and lack of awareness in the medical community has led to the battle patients, and Lipedema surgeons are currently fighting. We must educate and advocate for these surgeries to be covered.
When seeking treatment, women with lipedema are faced with two difficult decisions. First, they can pay out-out-pocket for the necessary surgeries and hope for reimbursement later. For women without access to these types of funds, it’s not an option at all. Otherwise, they must decide to put off treatment until their insurance provider agrees to cover the cost. More often than not, this process can take years, involves educating the insurance company on the medical seriousness of the disease and the necessity of treatment, and requires several levels of appeal. Some patients are lucky to find a partner and advocate in their healthcare provider, but the journey is long and arduous, even with a team behind them.
Will Medicare or Medicaid cover lipedema surgery?
No. Medicare and Medicaid do not cover cosmetic procedures. The only way lipedema treatment has been coded is under codes 15877, 15878, 15879. These three codes are for cosmetic liposuction procedures only. CMS (Center for Medicare and Medicaid) only accepts procedures with CPT codes. Lipedema reduction surgery does not have it’s own code. Instead, the insurance carriers are using the cosmetic codes 15877, 15878, 15879 to help providers understand how much a procedure will cost (and how much they need to cover).
Why are medical insurance carriers using cosmetic liposuction codes?
There is no specific CPT code for lipedema reduction, so medical insurers have chosen to use cosmetic codes, which makes treatment easier to deny. Cosmetic codes also have no assigned value, so they have no agreed-upon RVU (assigned value). So that means that insurers can pay whatever amount they want to pay for that procedure when they use the cosmetic code.
Even if medical insurance carriers agree to cover lipedema surgery, they can pay whatever they want to pay and are under no obligation to pay the appropriate amount to cover the cost of the surgery. Sometimes, they pay less than $200! As it stands, without an accurate CPT and RVU, carriers can pay whatever they want or whatever they think is fair. Today, they’re using codes based on cosmetic treatment, which is both inaccurate as a treatment and for cost. This has resulted in surgeons beings forced to go out of network and negotiate single-case agreements.
Why do medical insurance carriers not cover lipedema surgery?
But if I’ve been diagnosed with Lipedema, why won’t my medical insurance carrier cover treatment?
Essentially, medical insurance carriers disagree with the diagnosis and necessity for treatment. Even though your doctor and many doctors may diagnosis you with lipedema and say you may benefit from lipedema surgery, their doctors or reviewers can disagree. In addition to the above reasoning about covering poorly or denying coverage, an insurance provider can disagree with the diagnosis and/or that surgical treatment is necessary. Their determination of what is “impairing” a patient’s qualify of life is very different from what a patient with lipedema would confirm is impairing them. As a result, they deny surgical coverage. When looking at images of a patient with lipedema, providers have argued against lipedema and decided patients need to simply “lose weight” and diagnosed them with obesity, rather than their actual diagnosis of lipedema by their provider.
Why is lipedema surgery more expensive than traditional liposuction?
When you’re doing larger areas like lipedema, procedures are more prolonged, removing larger volumes than usual, and special care must be taken to care for the lymphatics. All of this must happen and is reflected in the average cost, but none is reflected without going out of network. Average liposuction is 1-2 hours and costs about $7000. Lipedema surgery is 4-5 hours and costs the provider about $10-$15k. Providers are doing this, but they are in hospital, and they can bill for staffing of ORs and overnight stays to cover the costs creatively. Unfortunately, this also results in the surgeon only providing 1-2 hours of surgery, so Lipedema patients suffer and see little to no improvement.
Are lawyers or advocates recommended to help get coverage?
We highly recommend speaking with your lipedema provider before working with lawyers or advocates. Unfortunately, some parties/people are predatory and charge large sums to help get these procedures covered but ultimately are unsuccessful. Patients have been scammed out of money with the promise they’d be reimbursed and wind up paying legal fees without ever being reimbursed for procedures.







