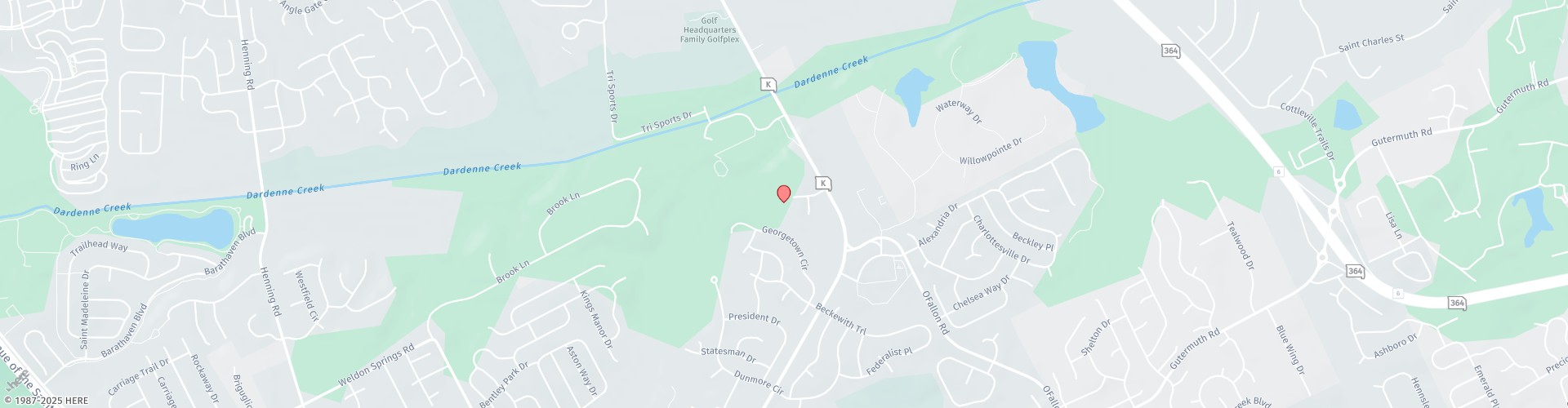
Modified liposuction surgery is the only available technique to correct and remove the abnormal adipose tissue of lipedema. Liposuction is a surgical treatment that involves the application of local (tumescent and water-assisted) anesthesia, and subsequent removal of adipose tissue through a straw-like device called a cannula. One end of the cannula is connected to a vacuum device, and the other end is inserted through a small incision of the skin and removes fat via aspiration. Learn more about lipedema lipo below!
There are two techniques of liposuction that can be safely used to treat lipedema, provided the surgeon has experience in techniques to avoid injury to the lymphatics. Note: Lipedema patients often have impaired lymphatic function, so great care must be taken to avoid further damage. The two liposuction techniques are safest and most effectively used by surgeons with a great deal of experience with the treatment of lipedema are tumescent liposuction and water-assisted liposuction. These two are the only research-backed surgical treatment plans for lipedema.
Tumescent Liposuction
involves the introduction of large volumes of tumescent solution into the fat below the skin space to tumesce (or swell) the area. This solution contains lidocaine anesthetic, which causes local numbness; epinephrine, which causes constriction of blood vessels to reduce the risk of bleeding; and saline, which causes swelling of the adipose tissue and protects the vascular structures from trauma. The solution is allowed to infiltrate the tissue, and its salinity causes the adipose tissue and cells to swell and separate from the connective tissue, at which point the cannula is used to aspirate the fat.
Water-Assisted Liposuction
does not involve over-swelling [tumescence] of the adipose tissue. Instead, small amounts of tumescent solution and water are introduced into the adipose tissue. Once sufficient numbing occurs, a modified cannula with an attached fan-shaped and slightly pressurized saltwater jet is inserted into the subcutaneous space and applied to separate the adipose cells from the tissue, while simultaneously aspirating the solution and detached cells.
When Should Liposuction Be Used to Treat Lipedema?
All the experts on lipedema agree that the timing of liposuction needs careful consideration. It is crucial for patients to be evaluated by a doctor who can fully diagnose and assess a patient before any consideration of surgery. The type and stage of lipedema need to be diagnosed, and a careful exam should be performed to detect swelling or secondary lymphedema.
Most patients have secondary swelling or lymphedema, which should be addressed with conservative measures prior to considering surgery- Be wary of surgeons who claim this not necessary. Most patients will benefit from compression, lymphedema therapy, and other conservative measures first. For the relatively few patients with early lipedema, no secondary swelling, or lymphedema, liposuction can be done without a lengthy conservative therapy. However, it is critical that proper physical assessment of swelling be done before surgery is considered. This keeps you, as the patient, safe, but it also provides other benefits. By focusing on conservative measures first, ideally only the most stubborn swelling and lipedema fat will remain, which can then be considered for surgery.
Non-Surgical Lipedema Therapy Before Liposuction
Lipedema experts and researched guidelines recommend a multidisciplinary approach to the new treatment for lipedema. This typically includes a lymphedema therapist, nutritional counseling, and compression instruction and fitting.
Lipedema is a chronic progressive congenital fat storage disorder that can affect the quality of life and health of the person with the disease. Some of the symptoms caused by lipedema—heaviness, pain, and secondary swelling—can be alleviated, at least in part, by conservative treatments such as compression or short stretch wraps, manual lymph drainage, and medication. However, there are several limitations to conservative treatments.
Conservative treatments afford temporary relief while they are practiced, but the effect of conservative treatments is variable. Some individuals experience significant relief, while others experience only very limited relief. Additionally, conservative treatments are not able to redress all symptoms. For example, conservative treatments have little to no effect on the mobility problems that occur as a result of the abnormal accumulation of fat around the knees or thighs, and conservative therapy is not able to address psychological or social issues resulting from the disproportionate body shape. Lastly, conservative therapy, as far as we can tell, is unable to halt the progression of lipedema.
There is some disagreement on how long conservative treatments should be practiced before considering treatments, which will vary by patient and surgeon. Some experts recommend the optimization of lymphatic flow with compression and therapy. However, the Dutch lipedema guidelines go further and state that “[liposuction] is only the treatment of choice for patients with a suitable health profile and/or inadequate response to conservative therapy. Before using [liposuction], associated deteriorating components such as edema, obesity, unhealthy lifestyle, lack of physical activity, lack of knowledge about the disease, and psychosocial distress should be addressed. Moreover, even after lipedema lipo, women generally require conservative therapy, and weight normalization should remain a goal.”
Lipedema Lipo Treatment
Unfortunately, there is no cure for lipedema. For many women, the most comprehensive way to treat the symptoms is lymph sparing liposuction. This surgical option is the only one that can remove the abnormal fat of lipedema; however, great care must be taken to spare lymphatic structures when performing lipedema lipo. Although not all people with lipedema suffer swelling of the limbs, many have abnormal lymphatic function [Harwood DOI: 10.1046/j].
There are two specialized lipedema lipo techniques that have been shown in studies to benefit individuals with lipedema: water-assisted and tumescent liposuction. In addition to the surgical equipment used, it is important to choose a surgeon with experience and one that is cautious when performing the surgery. These factors can have an important influence on protecting lymphatic flow and function.
Tumescent Liposuction vs. Water-Assisted Liposuction
Micro-cannula tumescent liposuction, performed with great care to avoid lymphatic injury, was shown to significantly improve pain, mobility, and leg size [Rapprich: “Liposuction is an Effective Treatment for Lipedema Results of a Study with 25 Patients”]. After the fat tissue is infused with a tumescent solution to swell the fat cells and constrict vessels, 3mm microcannulas are used to remove the lipedema fat by suction. This surgical technique has been shown to achieve long-lasting improvement in symptoms. Read more about this technique here.
Water Assisted Liposuction – similar to Body Jet Water Lipo [WAL, Aqua Shape, or Body Jet Lipo] has also been shown to produce significant improvement of mobility, symptoms, and quality of life factors for individuals with lipedema. Water Assisted Liposuction is similar to tumescent liposuction; however, the tumescent solution is pressurized to dislodge or loosen the fat from its surrounding connective tissue and vessels. Read more about this technique here.
In theory, the pressurized tumescent fluid should be gentler than traditional tumescent liposuction, but the final step for both requires a similarly shaped suction cannula. The ideal way to compare the relative safety and effectiveness of these two techniques would be a head-to-head study of both techniques where traditional tumescent liposuction using a micro-cannula lymph sparing technique was used on one leg and the WAL was used on the other leg. No head-to-head trial of the two techniques has been conducted.
At this time, most experts believe that both techniques, in the proper hands, are a safe and effective new treatment for lipedema, as long as the surgeon performing the liposuction has the skill and experience to perform a lymph sparing technique. We do know that traditional liposuction, without special care of the lymphatics or proper tumescent technique, can cause lymphatic damage and possibly worsen lipedema symptoms. [Hoffman Plast Reconstr Surg. 2004 Feb;113(2):718-24; discussion 725-6].
How to Decide if Lymph Sparing Liposuction Is Right for You
To be clear, lipedema lipo cannot cure lipedema – it can only provide fat reduction and symptom relief, and slow the progression of this disease. Liposuction is not an appropriate option for everyone with lipedema, and like any surgical procedure, there are risks.
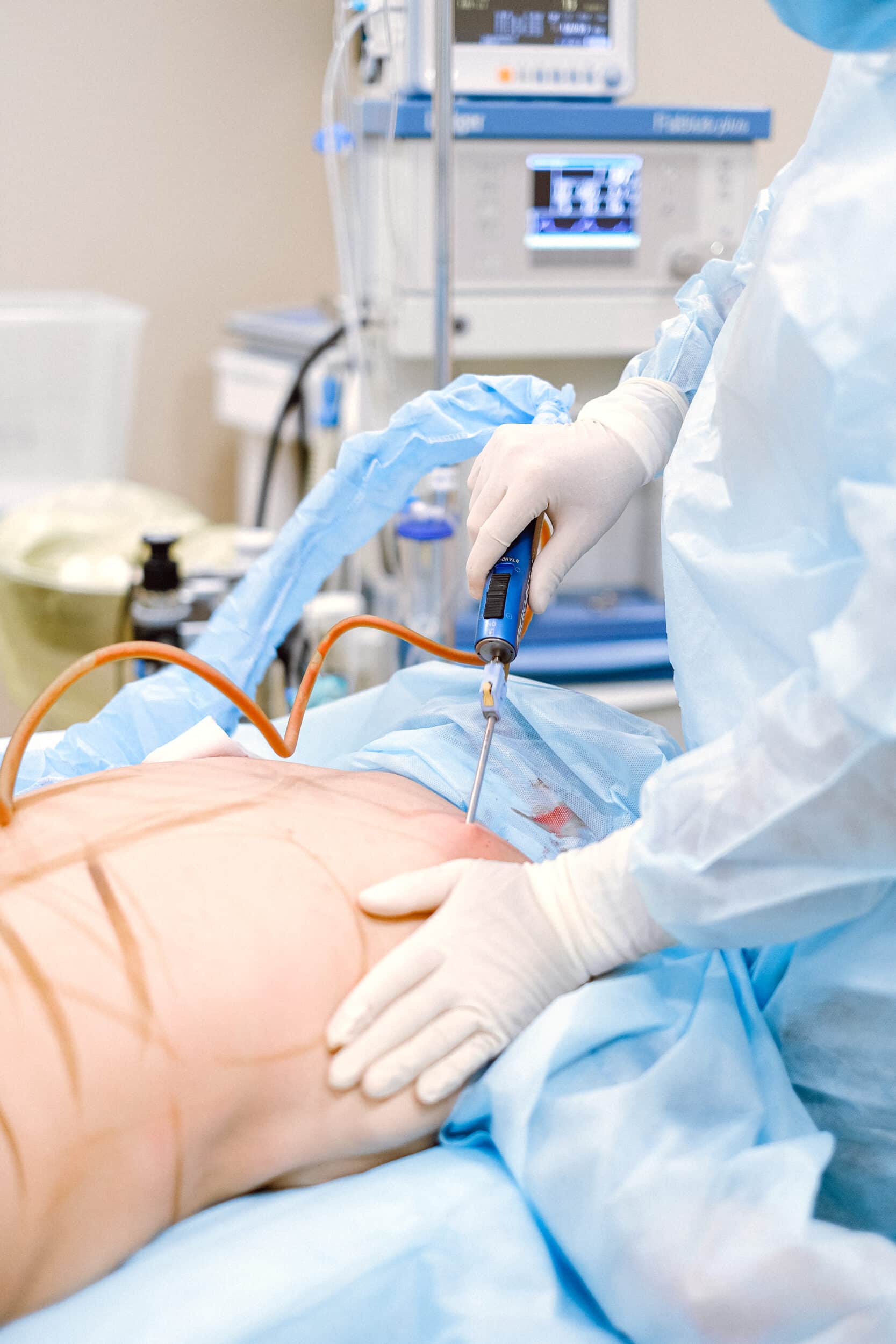
Although lipedema lipo is generally safe in healthy individuals, risks such as infection, bleeding, and trauma to the area may occur. Post-operative swelling in the limbs after surgery, which occurs with any lipedema lipo procedure, is more prolonged in individuals with lipedema. The swelling typically worsens for a few months before it gets better, and the full benefit may not be realized for six months to a year. However, overall, most patients with lipedema experience significant improvement of many or all of their symptoms, with varying individual results.
Although some people who have lipedema limited to only one specific area may need one procedure, most people undergo multiple lipedema lipo procedures to address all the different areas affected by lipedema. The multiple liposuction procedures need to be staged, or separated, to be done safely. The timing of the procedures depends on multiple factors, including the clinical stage of lipedema in the patient, the amount of fat being removed, the patient’s health and mobility, and other logistical factors.
Is Lipedema Lipo Surgery Covered by Insurance?
Lipedema is an inherited loose connective tissue and fat storage disease. Ideally, all treatments should be covered by medical insurance. But unfortunately, today’s reality is that still most medical insurance companies do not cover the cost of lipedema lipo for the treatment of lipedema and the few insurance providers that do cover the lipedema lipo treatment cover only a portion of the cost. However, things are changing and insurance coverage is beginning to improve.
Medical insurance only covers diseases that impact women’s daily lives and affect mobility and quality of life. Lipedema’s impact on people’s lives is variable. Some women have few symptoms caused by lipedema. However, for some women, lipedema affects their ability to walk, causes pain, swelling, and fatigue that limits the activities of their daily life and/or causes secondary complications that impact their lives. From a financial perspective, medical insurance companies either don’t want to cover lipedema or only cover lipedema that is causing symptoms that are severe enough to impact the person’s daily life and overall quality of life.
Usually, the diagnosis of lipedema alone will not persuade an insurance company that lymph sparing liposuction is medically necessary. Additional documentation from a multidisciplinary team of medical professionals lead by a knowledgeable doctor is the most effective way to persuade an insurance company to cover lipedema reduction surgery.
A recent survey showed that over 90% of doctors are not familiar with and do not recognize Lipedema in their patients. Finding a doctor who easily recognizes Lipedema, the types of Lipedema, the stages of Lipedema, and how Lipedema can impact your life is difficult.
When you’re diagnosed with Lipedema, it’s extremely important to not only have a thorough diagnosis of Lipedema in all the areas it is affecting, but also documentation of its impact on how it interferes with activities you do throughout the day.
The medical insurances that do cover the surgical treatment for Lipedema now often require documentation also adherence to the conservative, non-surgical treatments for Lipedema, such as medical-grade, graduated compression use, proper diet, and often lymphedema therapy.
For many women, Lipedema can make climbing and descending stairs difficult, can interfere with sitting in chairs, or lifting your arms over your head. If you are thinking about trying to get medical insurance to cover your lipedema surgery it is very helpful for your primary care doctor to write a letter explaining the medical reasons why he or she thinks the surgery will help you. It is also helpful to have the physical therapist and or occupational therapist you have seen for your treatment of lipedema provide notes. Also, it can be helpful for women with lipedema to write a letter documenting how the lipedema is interfering with her life.
A request for a new ICD-10 Diagnosis Code for Lipedema has been submitted. This effort was organized by Dr. Herbst, Dr. Shapira, and Dr. Wright and supported by American Venous and Lymphatic Society and Jeff Restuccio CPC. Nothing has been approved yet, but the request is making its way through the committee at the CDC. Also, we are happy to report that several health insurance providers now have medical policies in place to cover lipedema reduction surgery. The insurance providers are Aetna, Anthem, Blue Cross Blue Shield of Illinois, and Blue Cross Blue Shield of Michigan. The insurance providers all have medical necessity criteria which are too lengthy to list here, but they include documentation of lifestyle changes, including adherence to a prescribed diet, functional assessment by a physical or occupational therapist, and documentation of prescribed medical-grade graduated compression (minimum 20 – 30 mmHg).
Medical policy criteria require a 90-day follow-up with your physician to document adherence to the medical policy criteria. In general, most conservative therapy is covered by your health insurance. Out of pocket costs will apply if you have not met your deductible, you have a copay, and/or co-insurance. For many years, our office worked with insurance providers to obtain coverage for lipedema surgical procedures for our patients. In the last year, we decided to work through advocates because we thought the process would be faster and we would get more patients approved. We found that the use of an advocate was very costly for patients and the process interfered with continuity of care. Also, as most health insurance providers are adding medical policies to cover lipedema surgical procedures, the use of an advocate is usually unnecessary.
For these reasons, Dr. Wright is pleased to announce the addition of a full-time insurance coordinator to his team! This position is dedicated to working with patients to obtain approvals and get coverage for lipedema reduction surgery. In addition, she will also work with insurance to obtain single-payer agreements where necessary. We are pleased to be able to offer this service at no cost to our patients and we want you to know there will be no increase in the procedure cost. We are dedicated to helping our lipedema patients obtain coverage for their lipedema treatment and believe this will help us achieve this goal.
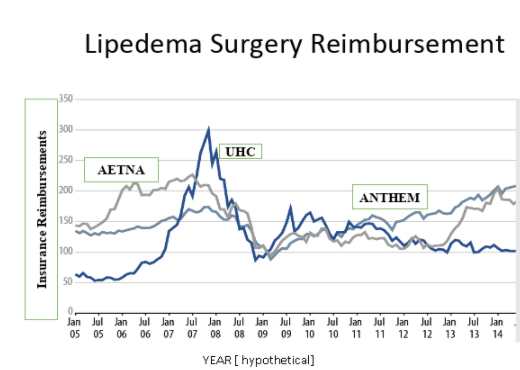
How can you find out if your medical insurance might cover lymph sparing liposuction as a treatment for your lipedema that is affecting your daily life? The first step is to contact your medical insurance company to see if they have a policy for covering surgery for lipedema. You can ask your insurance company if they have a patient advocate who can help insured patients get help with their medical problems.
Many companies and most larger employers have Human Resource or insurance company liaisons that can work as your advocate for insurance coverage for your lipedema. Women with lipedema have hired attorneys and advocates who have had some success in helping women with lipedema get coverage or reimbursements for lipedema surgery. There are attorneys and personal advocates that charge money and there are some that do not. It always pays to first find out if your insurance company will connect you with an advocate or your employer will connect you with an advocate. Local advocates who are familiar with your state’s medical insurer and their policies. Consumer reports, a respected consumer nonprofit organization, recommend looking for advocates through PatientAdvocate.org especially if your insurance claim is denied.
Another factor to consider is that most people must travel in order to get specific lipedema lipo. That means taking time off work, a helper/caregiver taking time off work to travel with you, and the expense of traveling and living for a while in another city. Medical insurance varies, but typically patients must front the costs and work with their provider on what they will be reimbursed if anything. However, whoever conducts your surgery should be able to provide you documentation necessary for filing a claim with your provider.
Lipedema Reduction Surgery: Recovery, Aftercare, & Maintenance

After Lipedema surgery, it’s important to understand that recovery takes months. In the first few weeks post-surgery, you are more swollen and tender. Recovery times depend on where the surgery was, how large the treatment was, and how much loose connective tissue and fat were removed.
For example, recovery from buttocks surgery can be aggravated because you have to sit on the affected area. Recovery from the lower legs is generally the hardest because this area is under the most pressure from the rest of the body. For this reason, it’s also typically one of the longest recovery times.
Strict adherence to compression is an absolute MUST to ensure proper healing and return of lymphatic function. Compression pumps, lymphatic massage, and other treatments that enhance lymphatic flow can greatly aid in the recovery from surgery. Even post-recovery, continued use of compression and adherence to these treatments can help maintain the results.
There are reports of a small percent of women who have had a recurrence of their symptoms of Lipedema in areas that were treated. We do not know, but it is very possible, that the recurrence may be prevented or lessened by continued maintenance of dietary and non-surgical treatments for Lipedema. The vast majority of women with lipedema experience improvement in pain, swelling, mobility, and quality of life from lipedema reduction surgery. However, because there is no cure for lipedema a healthy diet that emphasizes whole foods with limited processing especially limiting refined carbohydrates is important to maintain for the rest of your life.
What Non-Surgical Treatments are there for Lipedema?
The non-surgical, natural treatments for Lipedema are fortunately many, such as nutrition & supplements, exercise, lymph drainage & massage, compression, dry brushing & vibration and lymphatic yoga & breathing. You can learn more about each of them here.
Find more about the difference between inpatient vs outpatient liposuction here.
References:
- Rapprich, S., Dingler, A. & Podda, M. Liposuction is an effective treatment for lipedema-results of a study with 25 patients. J. Dtsch. Dermatol. Ges. J. Ger. Soc. Dermatol. JDDG 9, 33–40 (2011). https://www.ncbi.nlm.nih.gov/pubmed/21166777 or Google Scholar Link
- Buck, D. W. & Herbst, K. L. Lipedema: a relatively common disease with extremely common misconceptions. Plast. Reconstr. Surg. Glob. Open 4, e1043 (2016). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5055019/ or Google Scholar Link
- Schmeller, W., Hueppe, M. & Meier-Vollrath, I. Tumescent liposuction in lipoedema yields good longterm results. Br. J. Dermatol. 166, 161–168 (2012). Link https://www.ncbi.nlm.nih.gov/pubmed/21824127 and https://onlinelibrary.wiley.com/doi/full/10.1111/j.1365-2133.2011.10566.x or Google Scholar Link
- Wollina, U., Goldman, A. & Heinig, B. Microcannular tumescent liposuction in advanced lipedema and Dercum’s disease. G. Ital. Dermatol. E Venereol. Organo Uff. Soc. Ital. Dermatol. E Sifilogr. 145, 151–159 (2010). links https://www.ncbi.nlm.nih.gov/pubmed/20467389 and https://www.dovepress.com/treatment-of-elderly-patients-with-advanced-lipedema-a-combination-of–peer-reviewed-fulltext-article-CCID or Google Scholar Link
- Stutz, J. J. & Krahl, D. Water jet-assisted liposuction for patients with lipoedema: histologic and immunohistologic analysis of the aspirates of 30 lipoedema patients. Aesthetic Plast. Surg. 33, 153–162 (2009). Link: https://www.dovepress.com/lipedema-diagnostic-and-management-challenges-peer-reviewed-fulltext-article-IJWH or Google Scholar Link
- Damstra, RJ. First Dutch guidelines on lipedema using the international classification of functioning, disability and health. Phlebology. 2017 Apr;32(3):152-159. or Google Scholar Link
Dutch Standard of Care for Lipedema Guidelines: links https://journals.sagepub.com/doi/abs/10.1177/0268355516639421 and https://www.ncbi.nlm.nih.gov/pubmed/27075680