Lipedema is a chronic condition that affects many women, causing painful swelling in their legs and arms. The swelling can be so severe that it affects their mobility and quality of life. While there is no cure for Lipedema, there are ways to manage its symptoms. One of the most effective ways is to practice Lymphatic Yoga. This form of yoga is specifically designed to help stimulate the lymphatic system, which removes waste and toxins from the body.
By practicing Lymphatic Yoga, people with Lipedema can improve their circulation, reduce inflammation, and ease their pain. In this article, we’ll explore the benefits of Lymphatic Yoga for people with Lipedema and how it can be incorporated into their daily routine.
Lymphatic Yoga is a gentle form of yoga that involves fluid movements, breathing exercises, and mindfulness techniques. It is designed to stimulate the lymphatic system, which is crucial to our body’s immune system. The lymphatic system is a network of vessels and nodes that transport lymph, a clear fluid that contains white blood cells, throughout the body. The lymphatic system helps to remove waste, toxins, and excess fluid from the body. When the lymphatic system is not working properly, it can lead to a buildup of fluid in the tissues, causing swelling and inflammation.
Lymphatic Yoga helps to stimulate the lymphatic system by using gentle movements and deep breathing. The movements are designed to create a pumping action that helps to move the lymphatic fluid throughout the body. Deep breathing helps to increase oxygen levels in the body, which can also help to reduce inflammation. By practicing Lymphatic Yoga, people with Lipedema can improve their lymphatic flow, reduce swelling, and ease their pain.
Lipedema is a chronic condition that affects mostly women. It is characterized by the abnormal accumulation of fat and fluids in the legs, thighs, and buttocks. The swelling is usually symmetrical, meaning it affects both legs equally. Lipedema can also affect the arms and can cause pain, tenderness, and bruising. The exact cause of Lipedema is unknown, but it is thought to be related to hormonal imbalances and genetics.
Lipedema is often misdiagnosed or mistaken for obesity, leading to frustration and a delay in treatment. It is essential to recognize the symptoms of Lipedema and seek treatment early. Treatment options include compression therapy, manual lymphatic drainage, and Lymphatic Yoga.
Lymphatic Yoga can be an effective way to manage Lipedema symptoms. By stimulating the lymphatic system, Lymphatic Yoga can help to reduce swelling and inflammation. It can also improve circulation, which can help to reduce pain and discomfort. Lymphatic Yoga can be done at any time of the day and modified to suit individual needs and abilities.
The gentle movements and deep breathing of Lymphatic Yoga can help to stimulate the lymphatic system. The movements are designed to create a pumping action that helps to move the lymphatic fluid throughout the body. This can help to reduce the buildup of fluid in the tissues, which is a common symptom of Lipedema. Deep breathing can also help to increase oxygen levels in the body, which can help to reduce inflammation.
Several Lymphatic Yoga poses can be used to reduce swelling and pain associated with Lipedema. These poses are gentle and can be modified to suit individual needs and abilities.
Here are some Lymphatic Yoga poses that can be helpful for people with Lipedema:
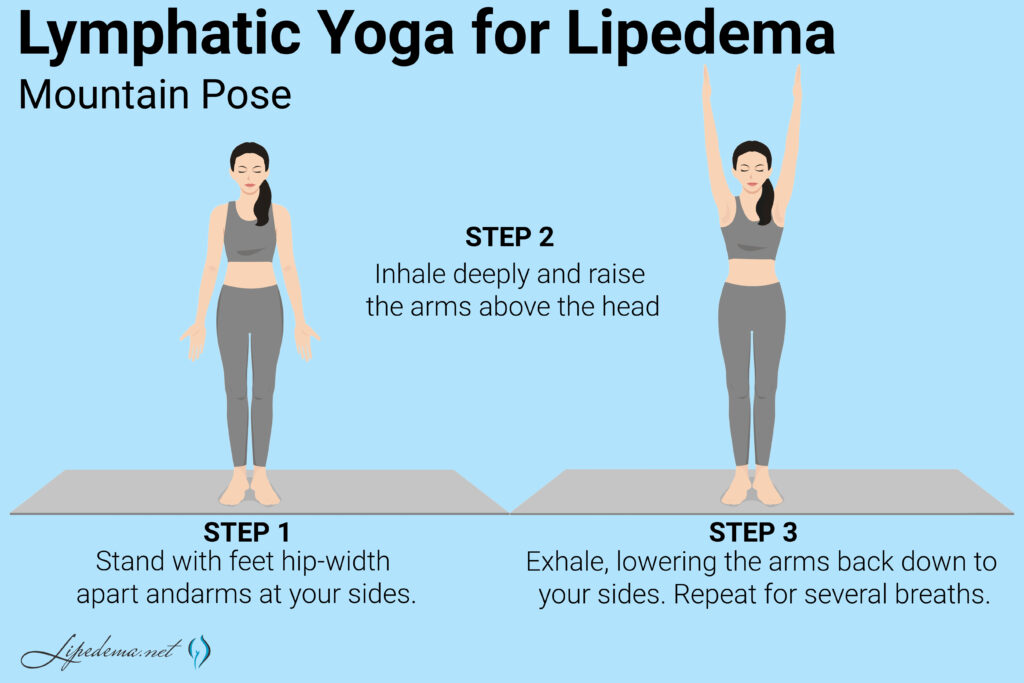

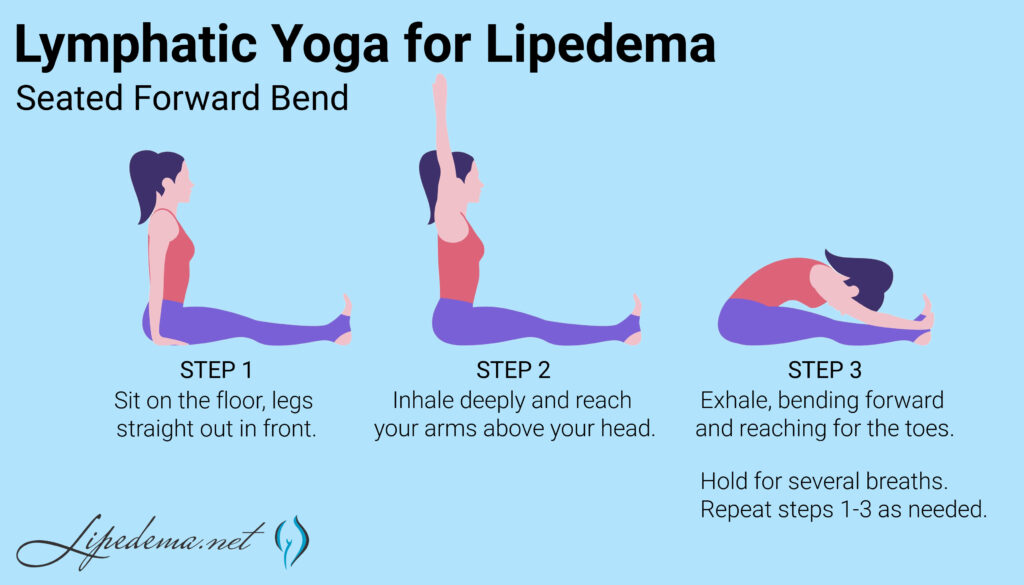





Lymphatic breathing techniques can be used to help improve lymphatic flow and reduce swelling. These techniques involve deep breathing and can be done at any time of the day.


Here are some lymphatic breathing techniques that can be helpful for people with Lipedema:
Lymphatic self-massage can be used to help improve lymphatic flow and reduce swelling. This technique involves gentle massage movements that help to move the lymphatic fluid throughout the body.
Here are some lymphatic self-massage techniques that can be helpful for people with Lipedema:
Incorporating Lymphatic Yoga into your daily routine can be a great way to manage Lipedema symptoms. Here are some tips for getting started:
In addition to Lymphatic Yoga, other natural remedies can help manage Lipedema symptoms.
These include:
Lipedema can be challenging to manage, but there are ways to reduce its symptoms. Lymphatic Yoga is a gentle and effective way to stimulate the lymphatic system, reduce inflammation, and ease pain associated with Lipedema. Incorporating Lymphatic Yoga into your daily routine can improve your lymphatic flow, reduce swelling, and improve your overall quality of life. Remember to start slow, be consistent, and listen to your body. With time and practice, you can find relief from your Lipedema symptoms and enjoy a more active and comfortable life.
Guidelines for the management of lipedema recommend the use of compression for patients with lipedema. The care guidelines recommend a multidisciplinary approach to treatment involving proper diet and exercise, manual lymphatic drainage, and wearing properly fitted, medical-grade compression garments. We’ve summarized everything women with Lipedema need to know about compression garments below, but you can find more information here.
What is Lipedema?
Lipedema is a fat disorder, mainly affecting women, that causes an enlargement of both legs due to deposits of fat under the skin. It’s characterized as a “progressive disorder,” meaning it generally gets worse over time. In severe and more progressive cases, the trunk and upper body may also be affected, including the arms and upper back, and it’s often misdiagnosed and incorrectly treated as general obesity.


Compression garments are used to help limit the swelling that occurs in Lipedema. This swelling contributes to the progression of lipedema, and can also lead to other painful and dangerous diseases.
Chronic swelling (also called “edema”) in the legs is a risk factor for eventually developing cellulitis and venous insufficiency and is one of the primary symptoms of lipedema. A recent study showed that swelling of the legs from any cause leads to an increased risk for leg skin infections or cellulitis. For women suffering from Lipedema, this can add insult to injury in an already debilitating disease accompanied by sensitive and easily bruised skin. If left untreated, cellulitis can move into the lymph nodes and bloodstream and require more serious medical treatment, and is one of many reasons why compression therapy for lipedema patients has more than one benefit!
For patients with Lipedema, there are many reasons to consider using compression garments or compression pumps. From clinical experience, it’s been noted that Lipedema and Lymphedema patients show faster and less complicated healing after surgery when patients are undergoing MLD/pump treatment before surgery. For individuals who have lipedema, lymphedema, or lipo-lymphedema, compression garments are often used to assist lymph circulation by increasing the pressure in the tissue to propel lymph fluid through the body. Lymphedema causes excess fluid to become trapped in the extremities, especially the legs, and compression garments pressure the skin and veins, helping them clear lymph and decongest. If we can utilize the garments to decrease the levels of chronic edema, we may also decrease the chances of developing cellulitis.


Compression garments can help reduce pain and heaviness felt in the limbs from fat disorders (such as lipedema) by decreasing swelling in the fat and throughout the limbs. Compression may also reduce the rate at which the fat cells grow and help to prevent fat disorders from progressing to more serious stages. In other words, compression can be one of the best treatments for lipo-lymphedema or fat caused by lymphatic diseases, in addition to cellulitis prevention.
Many patients don’t realize that edema (swelling) is just the beginning if untreated, and more severe conditions can occur. Skin infections, such as cellulitis, are more common in areas affected by lymphedema swelling than in normal skin, so women with lipedema have a higher likelihood of this condition. This is another reason compression therapy is imperative, whether you undergo surgery or not. If infections are not treated quickly, they may spread and become sepsis (blood poisoning or bacteremia), which can become fatal. Areas of long-term lymphedema swelling sometimes develop rare forms of cancer, such as lymphangiosarcoma or Stewart-Treves Syndrome (STS), that are frequently fatal. Any purple discoloration or tender nodules that develop on lymphedema-affected skin should be evaluated promptly by a medical professional.
Today, most doctors recommend conservative and preventative measures to keep you, such as daily washing of wounds or cuts that bacteria could infiltrate and applying protective creams, ointments, and bandages when necessary to surface damage or dehydrated, flaky skin. Preventative medications, such as antibiotics, may be recommended when patients experience several recurrences of cellulitis.
For people with poor circulation – such as diabetics or women with Lipedema and or Lymphedema, additional precautions for avoiding skin injury are recommended, but overall are still conservative and focus on healthy and consistent skincare. For example, the health providers at the Mayo Clinic recommend you inspect your feet daily, check for signs of injury or infection early on, moisturize skin regularly to avoid dryness or cracks, and trim fingers and toenails with great care to avoid injuring the skin and wear clean and protective footwear and gloves often.
Like Lipedema, there’s a lot we still don’t know about cellulitis; we know it can be caused by several types of bacteria infecting deeper layers of the skin, and we know that it causes swollen, red, painful areas in the skin. We know it commonly affects the feet and lower legs. But we don’t know how the bacteria get into the body of many people affected. And new studies suggest something else we did not know previously – compression therapy may help prevent this painful condition.

A recent study by the New England Journal of Medicine divided 84 patients into two groups. Participants in each group experienced chronic swelling in their legs and also suffered from cellulitis on an ongoing basis. In the first group, participants received compression therapy and were provided education on how to prevent their cellulitis from returning. In the second group, participants received the same education but did not undergo compression therapy. The groups returned for follow-up therapy and education every six months for up to three years, until the entire trial experienced a total of 45 cases of cellulitis. When someone in group two experienced a return of their cellulitis, they were moved to group one to under compression therapy.
Overall, the quality of life in both groups was the same, and there weren’t drastically different experiences between groups one and two. However, the group who received therapy and cellulitis prevention education experienced only 6 new cases of cellulitis, while the second group experienced 17 cases. While the study was small, and additional studies are needed, early indications suggest compression therapy will result in a lower recurrence of cellulitis than education and conservative treatments alone. We have known for years that people with lymphedema have an increased risk for cellulitis, and they benefit from compression. However, this study showed leg swelling from any cause puts affected individuals at risk for infections, and compression helps reduce this risk.
It’s essential that compression garments are appropriately measured to ensure they fit correctly. Incorrectly fitted compression can be painful and even make lipedema symptoms worse! Most cities have a medical supply store that will measure you and then help you find the appropriate garments, but if you’re ordering them online, you’ll have to measure yourself by following their guidelines. For online orders, we recommend https://www.brightlifedirect.com/ and https://www.compressionguru.com/.
Ready to Learn More about Lipedema Surgery in St. Louis? Let’s Chat!
Still not sure where to start? That’s okay! Physicians such as Dr. Wright can provide you with the needed treatment plans that it takes to reduce your lipedema symptoms. Contact us today!
Chronic swelling (also referred to as “edema”) in the legs is a risk factor for eventually developing cellulitis, venous insufficiency, and is one of the primary symptoms of lipedema. A recent study showed that swelling of the legs from any cause leads to an increased risk for leg skin infections or cellulitis. For women suffering from Lipedema, this can add insult to injury in an already debilitating disease accompanied by sensitive and easily bruised skin. If left untreated, cellulitis can move into the lymph nodes and bloodstream and require more serious medical treatment, and is one of many reasons why compression therapy for lipedema patients has more than one benefit!
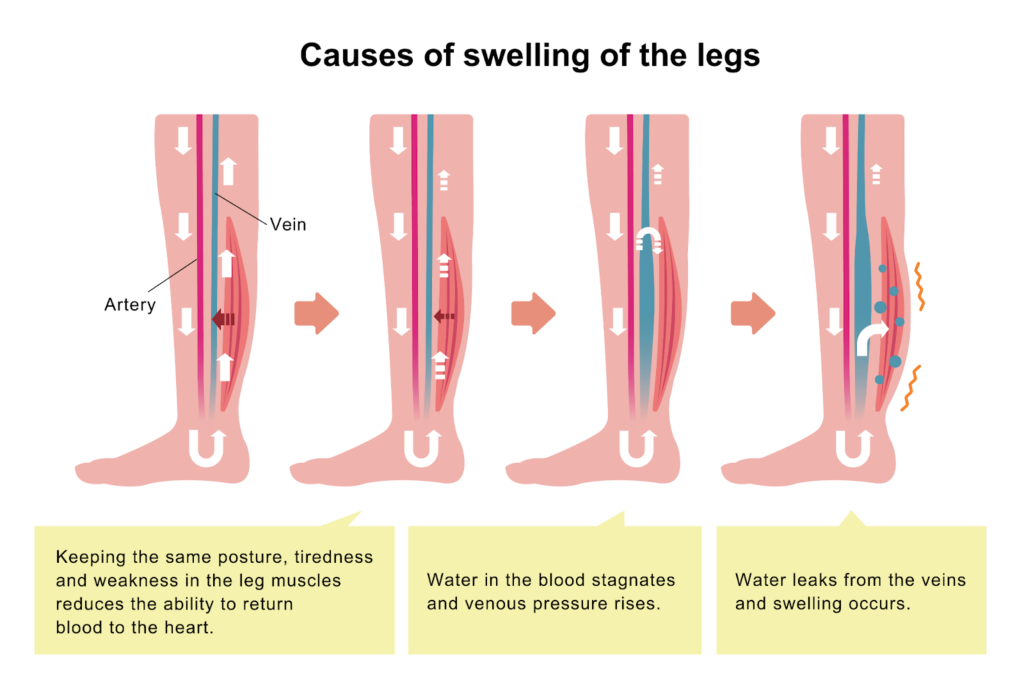

Today, most doctors recommend conservative and preventative measures, such as daily washing of wounds or cuts that could be infiltrated by bacteria, and the application of protective creams, ointments, and bandages when necessary to surface wounds or extremely dry, flaky skin. Preventative medications, such as antibiotics, may be recommended in some instances where patients experience several recurrences of cellulitis.

For people with poor circulation – such as diabetics or women with Lipedema or Lymphedema, additional precautions for avoiding skin injury are recommended, but overall are still conservative and focus on healthy and consistent skincare. For example, the health providers at the Mayo Clinic recommend you inspect your feet daily, check for signs of injury or infection early on, moisturize skin regularly to avoid dryness or cracks, trim finger and toenails with great care to avoid injuring the skin and wear clean and protective footwear and gloves often.
Like Lipedema, there’s a lot we still don’t know about cellulitis; we know it can be caused by several types of bacteria infecting deeper layers of the skin, we know that it causes swollen, red, painful areas in the skin, and we know it commonly affects the feet and lower legs. But we don’t know how the bacteria get into the body for many people affected. And new studies suggest something else we did not know previously – compression therapy may help prevent this painful condition.
A recent study by the New England Journal of Medicine divided 84 patients into two groups. Participants in each group experienced chronic swelling in their legs, and also suffered from cellulitis on an ongoing basis. In the first group, participants received compression therapy and were provided education on how to prevent their cellulitis from returning. In the second group, participants received the same education but did not undergo compression therapy. The groups returned for follow-up therapy and education every six months, for up to three years, until the entire trial experienced a total of 45 cases of cellulitis. When someone in group two experienced a return of their cellulitis, they were moved to group one to under compression therapy.
Overall, the quality of life in both groups was the same, and there weren’t drastically different experiences between group one and group two. However, the group who received both therapy and cellulitis prevention education experienced only 6 new cases of cellulitis, while the second group experienced 17 cases. While the study was small, and additional studies are needed, early indications suggest compression therapy will result in a lower recurrence of cellulitis than education and conservative treatments alone. We have known for years that people with lymphedema have an increased risk for cellulitis and they benefit from compression. However, this study showed leg swelling from any cause puts affected individuals at risk for infections, and compression helps reduce this risk.


For patients with Lipedema, there are many reasons to consider using compression garments or compression pumps. From clinical experience, it’s been noted that Lipedema and Lymphedema patients show faster and less complicated healing after surgery when patients are undergoing MLD/pump treatment before surgery. For individuals who have lipedema, lymphedema, or lipo-lymphedema, compression garments are often used to assist lymph circulation by increasing the pressure in the tissue to propel lymph fluid through the body. Lymphedema causes excess fluid to become trapped in the extremities, especially the legs, and compression garments put pressure on the skin and veins, helping them clear lymph and decongest. If we can utilize the garments to decrease the levels of chronic edema, we may also decrease the chances of developing cellulitis.
Compression garments can help reduce pain and heaviness felt in the limbs from fat disorders (such as lipedema) by decreasing swelling in the fat and throughout the limbs. Compression may also reduce the rate at which the fat cells grow, and help to prevent fat disorders from progressing to more serious stages. In other words, compression can be one of the best treatments for lipo-lymphedema or fat caused by lymphatic diseases, in addition to cellulitis prevention.

Another option patients have to manage their own symptoms at home is pneumatic compression pumps. Pneumatic compression pumps are a great at-home solution for patients suffering from lipedema or lymphedema, and potentially for cellulitis prevention. Compression pumps are devices that mimic the massage techniques used in manual lymphatic drainage. An intermittent pneumatic compression device (IPC) is worn on the affected limb and activated to help push retained fluids back towards the core of the body. These devices let patients who may have difficulty or are unable to visit a doctor’s office often still find relief from their symptoms.
If you have compression stockings but aren’t providing enough relief, an intermittent pneumatic compression device can help you get daily treatment. These treatments are very effective at treating extreme levels of swelling, and IPC devices help patients to continue their treatment at home and keep their lymph fluid from rebuilding in the affected limbs. As we continue to monitor the development and new studies related to how these practices may help prevent the recurrence of cellulitis, we will update the data here as well. Contact us today!
One of the most common symptoms of lipedema that is observed in all stages is swelling. This symptom is due to an increased amount of extracellular water causing the swelling. This extracellular water is lymphatic fluid that contains hundreds of inflammatory compounds that are responsible for fibrosis that drives the progression of lipedema. The increase of water will only increase with each further stage. One of the most frequently recommended forms of care for swelling and pain is wearing compression garments. This step in our multidisciplinary approach is typically recommended in the first stage but always in later stages.
The specific goals for wearing compression garments is to reduce any discomfort and aching that your swelling is causing. Compression has an anti-inflammatory effect on the tissue by reducing interstitial fluid formation and ensuring fluids are kept moving to reduce lymphatic stasis. Compression therapy can also help your limb improve its movement and reduce edema. Finally, compression can help smooth out lobules and cuffs caused by lipedema.
We understand that that the lymphatic system plays a critical role in how lipedema progresses. Medical grade compression stockings are prescribed during treatment and have been observed to treat the symptoms of lipedema and promote lymphatic flow. Wearing compression garments can help prevent excess interstitial fluid that is directly linked with nodular fibrosis and lobular fibrosis. These fibrotic processes are also linked to eventual disability stemmed from lipedema.
The prescribed compression garment is dependent on the individual needs of your lipedema. It is important the compression is graduated to promote lymphatic fluid movement. These garments apply 100% compression strength to the distal end of the limb worn on your ankle or wrist. The compression garment gives gradually decreased percent of compression as it goes more proximally toward the center of your body and heart. Typically, our arms require less compression strength than our legs do. Most physicians will start out prescribing a lower graduated compression before working up to a heavier progression. A recommended graduated 30-40 mmHg pressure at the ankle and 18 mm Hg at the wrist has been shown to minimize edema, reduce symptoms, and halt the progression of diseases related to lipedema and lymphedema. Please note some compression sold is not graduated and is not medical grade. For example, Bioflect and Marena sell popular compression garments that are not graduated and are not medical grade. There is no evidence that Bioflect or Marena garments will have the desired effects. Sigvaris, Juzo, Jobst, and Solidea all sell graduated compression that have been shown to have the desired effects.
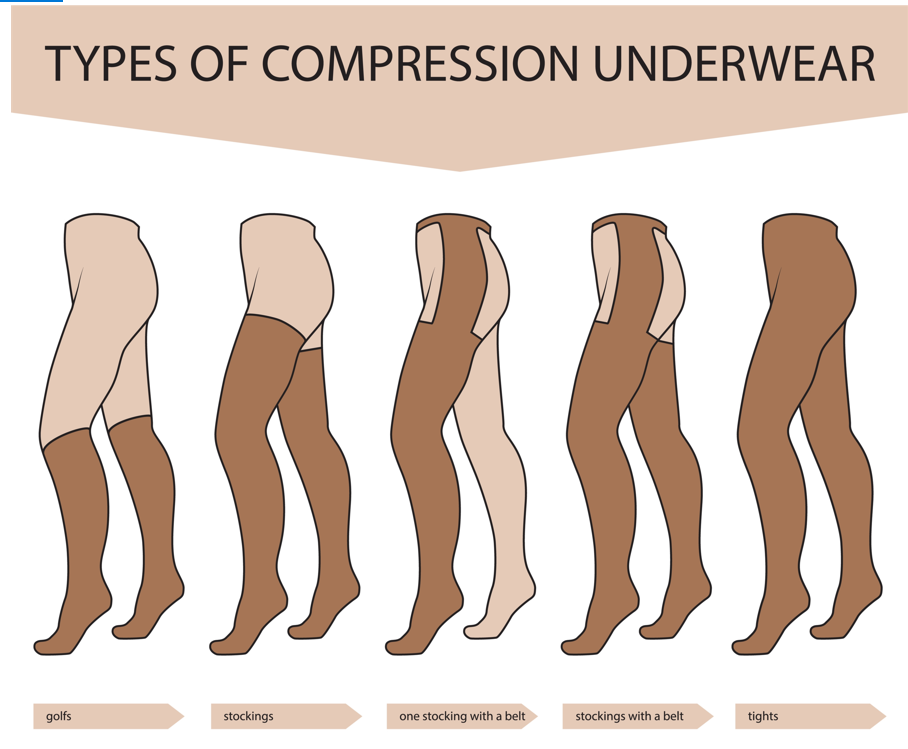
While compression garments are great, they can be difficult to fit on women with lipedema. As the fat accumulates out of proportion to the body, lipedema will lead to unique body shapes. In order to fit these shapes and allow individuals to remain flexible they will need to wear layering compression garments. These combinations can be seen as knee-high socks with compression pants. This allows the individual to have a comprehensive coverage without any gaps of compression. Contact us now!
Currently, most of the supplies needed to manage lipedema and lymphedema are not covered by Medicare. Compression garments, donning devices and wraps, which are critical for the proper care and management of these diseases are not covered except when caused by cancer treatment. These garments are quite expensive and need to be replaced as often as every six months. The lymphedema can be just devastating when caused by an inherited condition as is the case of lipedema or an infection. If lymphedema is not properly controlled by compression garments it progress and spiral into a progressively disabling condition.
The Lymphedema Treatment act will improve coverage for lymphedema from any cause from Medicare. Other insurance will follow Medicare lead. This legislation is critical for improving the health and lives of patients who suffer from lymphedema. There is much to do. Please follow these links to learn how you can contact your representative in the US Congress and Senate. Also, learn how to promote awareness for this important cause through social media.