

Lipedema is a fat disorder that mainly affects women and causes enlargement of both legs due to fat deposits under the skin. It’s characterized as a “progressive disorder,” meaning it worsens over time. In severe and more progressive cases, the trunk and upper body may also be affected, including the arms and upper back, and it’s often misdiagnosed and incorrectly treated as general obesity. While the exact prevalence of lipedema is still not well-known, estimates suggest that it may affect a significant portion of the female population. Below, we explore the lipedema prevalence and its symptoms, causes, and available treatment options.
Lipedema is a condition that often goes undiagnosed or misdiagnosed due to its similarity to other conditions, such as obesity and lymphedema. It typically begins during or after puberty, pregnancy, or menopause, suggesting a hormonal influence on its development. Lipedema is characterized by an irregular distribution of fat beneath the skin, causing the affected areas to become larger than other body parts. The condition primarily affects the legs but can also involve the arms in some cases. Unlike obesity, lipedema does not respond to traditional weight loss methods, making it distinct from lifestyle-induced weight gain. Additionally, lipedema is different from lymphedema as it does not start in the lower legs but rather affects the upper legs.
Lipedema is a connective tissue disease that may affect 6-19% of women. (1, 2, 3) If these numbers are valid and applied to the US population, millions of women in the US have lipedema.
Determining the exact prevalence of lipedema has been challenging due to the lack of awareness and recognition of the condition among healthcare professionals. However, recent studies and clinical observations have shed light on its prevalence. According to estimates, lipedema may affect approximately 1 in 9 women globally. This suggests that it is more common than previously believed. However, it is essential to note that the prevalence may vary depending on geographical location and the population studied.
In one study conducted in a referral clinic in Germany, it was found that approximately 11% of women and individuals assigned female at birth had lipedema. This estimate is higher than previous studies and highlights the need for increased awareness and understanding of the condition. However, it is essential to acknowledge that lipedema can be underdiagnosed or misdiagnosed, as it often resembles other conditions.


Lipedema is characterized by specific symptoms that differentiate it from other conditions. The most noticeable symptom is the disproportionate enlargement of the lower body, particularly the legs, hips, and buttocks. This irregular fat distribution can give the appearance of two different bodies combined, with a smaller upper body and a significantly larger lower body. The affected areas may exhibit a lumpy or nodular texture, and the skin may bruise easily. Individuals with lipedema may also experience pain, tenderness, and a heavy feeling in their legs. Other symptoms can include swelling, fatigue, and the development of spider veins or varicose veins in the legs.
It is important to note that lipedema can have a significant impact on an individual’s physical and emotional well-being. The appearance of the legs and the challenges in finding appropriately fitting clothes can lead to self-esteem issues, social isolation, and psychological distress. Therefore, early recognition and appropriate management of lipedema are crucial for improving the quality of life for affected individuals.
The exact cause of lipedema is still unknown, but several factors may contribute to its development. Hormonal influences are believed to play a role, as lipedema often starts or worsens during hormonal changes such as puberty, pregnancy, and menopause. Hormonal contraceptives, such as birth control pills, may also be a contributing factor. Additionally, there is evidence to suggest a genetic component to lipedema, as it tends to run in families.
While obesity itself does not cause lipedema, there is a correlation between the two conditions. It is estimated that more than 50% of individuals with lipedema have a body mass index (BMI) higher than 35. However, it is important to note that lipedema cannot be attributed solely to excess weight, as it is a distinct medical condition with unique characteristics.
Certain risk factors may increase the likelihood of developing lipedema. Being assigned female at birth, having a family history of lipedema, and having a BMI higher than 35 are factors associated with a higher risk of developing the condition.

Diagnosing lipedema can be challenging due to its resemblance to other conditions and the lack of awareness among healthcare professionals. A thorough medical history, physical examination, and evaluation of symptoms are essential for accurate diagnosis. Painful fat deposits and the presence of a significant difference in size between unaffected feet and affected legs can be indicative of lipedema.
There is no specific diagnostic test for lipedema. Still, imaging studies, such as ultrasound, DEXA scan, magnetic resonance imaging (MRI), computed tomography (CT), or nuclear medicine imaging, may be utilized to rule out other conditions or identify any associated complications. These tests can help in differentiating lipedema from conditions such as lymphedema and assessing the extent of fat deposition.
While there is no cure for lipedema, various treatment options are available to manage the symptoms and improve the quality of life for individuals with the condition. The treatment approach may vary depending on the severity of symptoms and individual needs.
Compression therapy, involving the use of compression garments or bandages, is commonly recommended to reduce swelling and provide support to the affected areas. Physical and occupational therapy, including manual lymphatic drainage therapy, can help improve mobility, reduce fluid buildup, and enhance overall well-being. Dietary changes, such as adopting an anti-inflammatory diet, may help manage symptoms and reduce the progression of lipedema. Strength and conditioning exercises, particularly low-impact activities like water exercise, can improve circulation, increase mobility, and promote overall fitness. Counseling or therapy may be beneficial for individuals with lipedema to address the psychological impact of the condition, including depression, low self-esteem, and body image concerns. Additionally, liposuction performed by specialized surgeons can be considered in select cases to remove the diseased lipedema fat and improve mobility and quality of life.
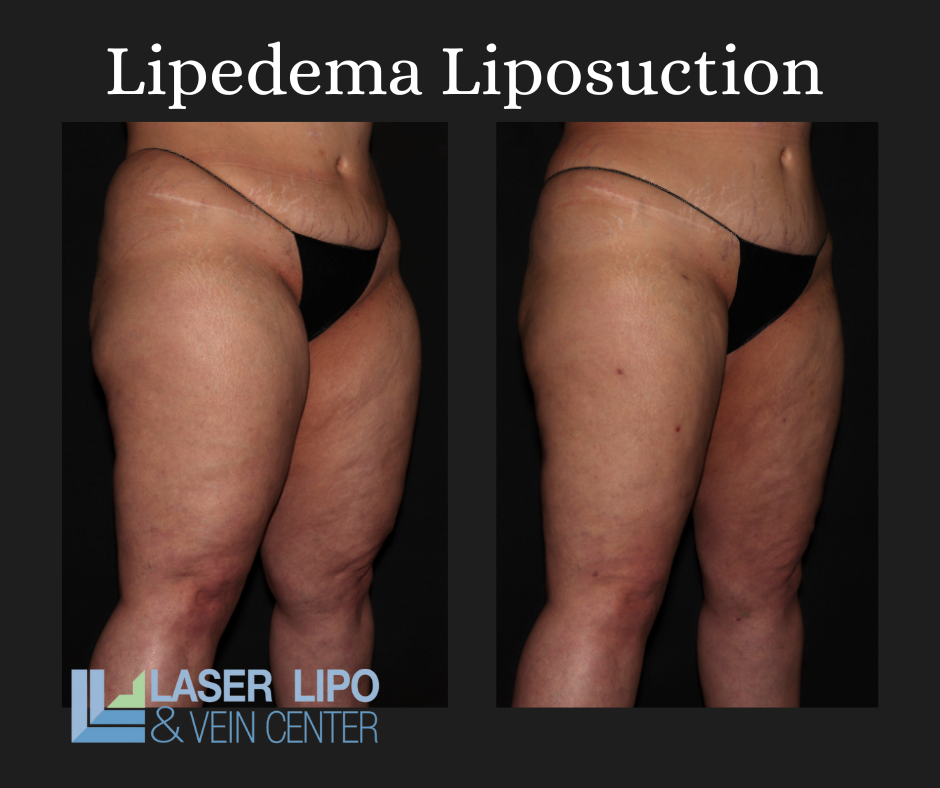

Ultimately, effective treatment will require surgical intervention to alleviate the appearance and pain of symptoms. Liposuction performed on the affected limbs is generally the most effective treatment. Removing diseased fat deposits helps reduce swelling of the limbs and alleviates the pain that holds patients back from everyday activities. This surgical treatment can provide various benefits and relieve the symptoms you are experiencing from lipedema. Dealing with lipedema can be difficult, especially if you are just now starting to take control of it. Lipedema reduction surgery is different from cosmetic liposuction. Studies have shown that women with Lipedema have impaired lymphatic function. Lymphatic fluid promotes the growth of more fat cells, which can overwhelm the lymphatic capillaries (branch-like blood vessels). Extra care must be taken to avoid injuring the lymphatic system and worsening an already stressed system. Studies have shown that lymphatic function can improve after this type of liposuction in women with Lipedema using blunt cannulas, generous tumescent anesthesia, and special surgical techniques. Lipedema reduction surgery aims to remove the fibrous tissue and maximally reduce the lipedema tissue. It is a “debulking” surgery, not a cosmetic surgery.


If you suspect that you may have lipedema, it is important to consult with a healthcare professional who specializes in the condition. A vascular surgeon, plastic surgeon, or dermatologist with expertise in lipedema can provide an accurate diagnosis and recommend appropriate treatment options based on your needs. Early diagnosis and management of lipedema are crucial in preventing the condition’s progression and improving overall health outcomes. By seeking professional help, individuals with lipedema can receive the care and support they need to manage their symptoms and maintain their quality of life. Lipedema is a prevalent condition that primarily affects women, causing abnormal fat buildup in the lower body. While the exact prevalence of lipedema is still uncertain, estimates suggest that a significant portion of the female population may be affected. Recognizing the symptoms, understanding the causes and risk factors, and seeking appropriate treatment are essential for managing lipedema and improving overall well-being. By increasing awareness and understanding of the condition, we can ensure that individuals with lipedema receive the care and support they deserve.
Sources
[i] Foldi E, Foldi M. Das lipodem. In: M Foldi, E Foldi, and S Kubik, eds. Lehrbuch der
Lymphologie für Mediziner, Masseure und Physiotherapeuten. Munich: Elsevier, Urban &
Fischer;2005:443-453.
https://www.amazon.com/F%C3%B6ldis-Textbook-Lymphology-Physicians-Lymphedema/dp/0723436460
[ii] Crescenzi R. Donahue PMC, Weakley S, Garza M, Donahue MJ, Herbst KL.
Lipedema and Dercum’s disease: a new application of bioimpedance. Lymphat Res
Biol 2019;17(6):671-679.
https://pubmed.ncbi.nlm.nih.gov/31408408/
[iii] Gould DJ, El-Sabawi B, Goel P, Badash I, Colletti P, Patel KM. Uncovering lymphatic
transport abnormalities in patients with primary lipedema. J Reconst
Microsurg 2020;36(2):136-141.
https://pubmed.ncbi.nlm.nih.gov/31546262/
Lipedema is a chronic condition that affects many women, causing painful swelling in their legs and arms. The swelling can be so severe that it affects their mobility and quality of life. While there is no cure for Lipedema, there are ways to manage its symptoms. One of the most effective ways is to practice Lymphatic Yoga. This form of yoga is specifically designed to help stimulate the lymphatic system, which removes waste and toxins from the body.
By practicing Lymphatic Yoga, people with Lipedema can improve their circulation, reduce inflammation, and ease their pain. In this article, we’ll explore the benefits of Lymphatic Yoga for people with Lipedema and how it can be incorporated into their daily routine.
Lymphatic Yoga is a gentle form of yoga that involves fluid movements, breathing exercises, and mindfulness techniques. It is designed to stimulate the lymphatic system, which is crucial to our body’s immune system. The lymphatic system is a network of vessels and nodes that transport lymph, a clear fluid that contains white blood cells, throughout the body. The lymphatic system helps to remove waste, toxins, and excess fluid from the body. When the lymphatic system is not working properly, it can lead to a buildup of fluid in the tissues, causing swelling and inflammation.
Lymphatic Yoga helps to stimulate the lymphatic system by using gentle movements and deep breathing. The movements are designed to create a pumping action that helps to move the lymphatic fluid throughout the body. Deep breathing helps to increase oxygen levels in the body, which can also help to reduce inflammation. By practicing Lymphatic Yoga, people with Lipedema can improve their lymphatic flow, reduce swelling, and ease their pain.
Lipedema is a chronic condition that affects mostly women. It is characterized by the abnormal accumulation of fat and fluids in the legs, thighs, and buttocks. The swelling is usually symmetrical, meaning it affects both legs equally. Lipedema can also affect the arms and can cause pain, tenderness, and bruising. The exact cause of Lipedema is unknown, but it is thought to be related to hormonal imbalances and genetics.
Lipedema is often misdiagnosed or mistaken for obesity, leading to frustration and a delay in treatment. It is essential to recognize the symptoms of Lipedema and seek treatment early. Treatment options include compression therapy, manual lymphatic drainage, and Lymphatic Yoga.
Lymphatic Yoga can be an effective way to manage Lipedema symptoms. By stimulating the lymphatic system, Lymphatic Yoga can help to reduce swelling and inflammation. It can also improve circulation, which can help to reduce pain and discomfort. Lymphatic Yoga can be done at any time of the day and modified to suit individual needs and abilities.
The gentle movements and deep breathing of Lymphatic Yoga can help to stimulate the lymphatic system. The movements are designed to create a pumping action that helps to move the lymphatic fluid throughout the body. This can help to reduce the buildup of fluid in the tissues, which is a common symptom of Lipedema. Deep breathing can also help to increase oxygen levels in the body, which can help to reduce inflammation.
Several Lymphatic Yoga poses can be used to reduce swelling and pain associated with Lipedema. These poses are gentle and can be modified to suit individual needs and abilities.
Here are some Lymphatic Yoga poses that can be helpful for people with Lipedema:
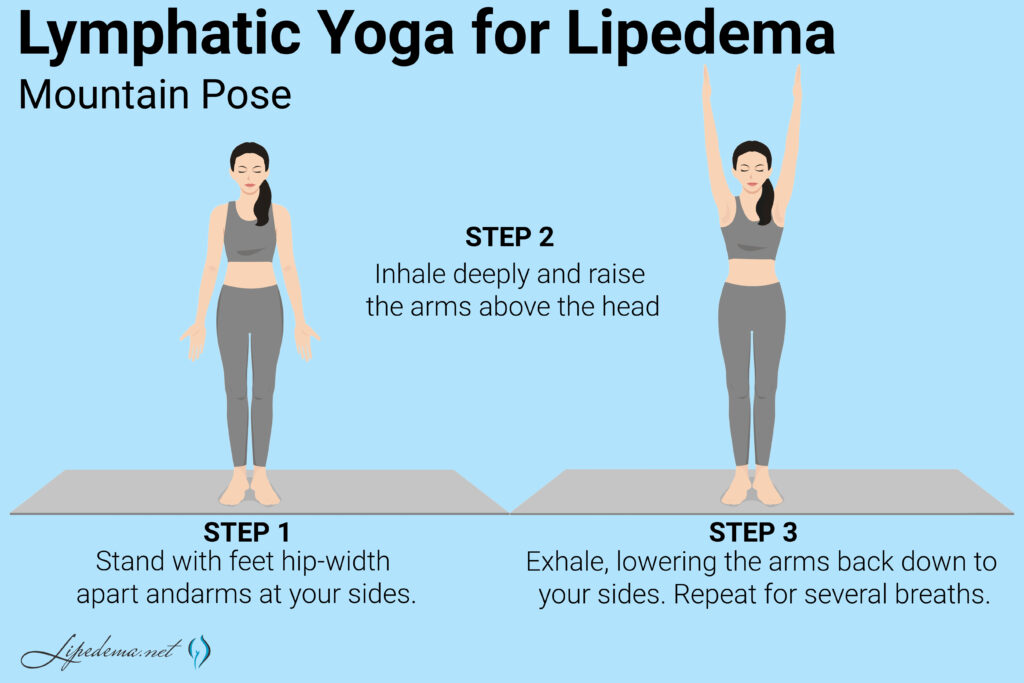

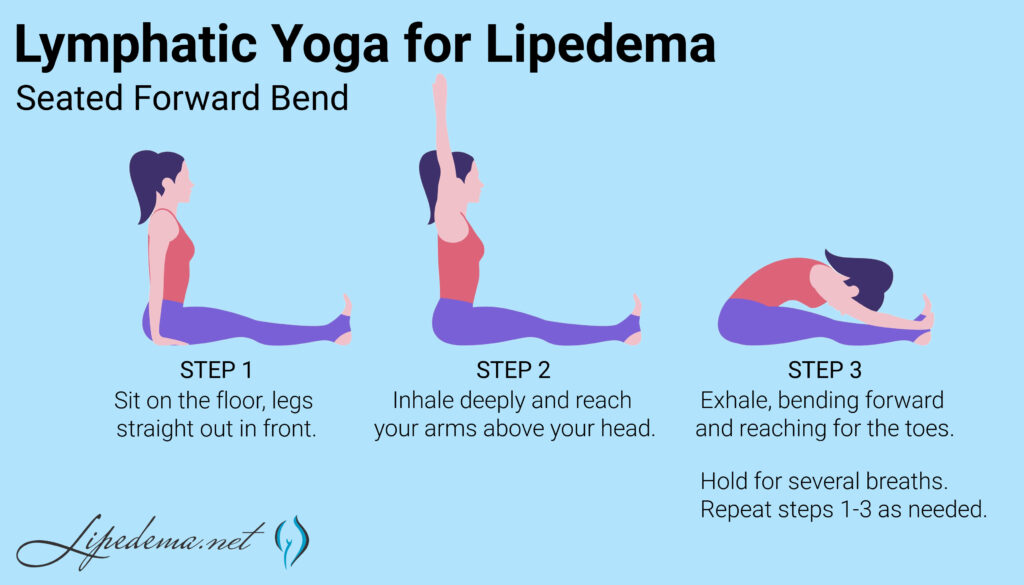





Lymphatic breathing techniques can be used to help improve lymphatic flow and reduce swelling. These techniques involve deep breathing and can be done at any time of the day.


Here are some lymphatic breathing techniques that can be helpful for people with Lipedema:
Lymphatic self-massage can be used to help improve lymphatic flow and reduce swelling. This technique involves gentle massage movements that help to move the lymphatic fluid throughout the body.
Here are some lymphatic self-massage techniques that can be helpful for people with Lipedema:
Incorporating Lymphatic Yoga into your daily routine can be a great way to manage Lipedema symptoms. Here are some tips for getting started:
In addition to Lymphatic Yoga, other natural remedies can help manage Lipedema symptoms.
These include:
Lipedema can be challenging to manage, but there are ways to reduce its symptoms. Lymphatic Yoga is a gentle and effective way to stimulate the lymphatic system, reduce inflammation, and ease pain associated with Lipedema. Incorporating Lymphatic Yoga into your daily routine can improve your lymphatic flow, reduce swelling, and improve your overall quality of life. Remember to start slow, be consistent, and listen to your body. With time and practice, you can find relief from your Lipedema symptoms and enjoy a more active and comfortable life.
Back pain is a common problem that affects many people. But for those who suffer from lipedema, it can be much more than just an annoyance. Lipedema is a chronic condition that causes painful swelling in the legs and buttocks. Fortunately, there is a life-changing solution – lipedema surgery.
In this article, we will explore what lipedema is, its symptoms, causes, diagnosis, and treatment. We will also discuss the different types of lipedema surgery and the benefits of undergoing this procedure. Plus, we’ll look at the recovery process and the success stories of those who have gone through it themselves.


Lipedema is a condition that primarily affects women and is characterized by painful swelling of the legs and buttocks. It is known as a “painful fat disorder” because it causes fat to accumulate in the lower body, leading to discomfort and difficulty moving.
Lipedema can be difficult to diagnose because its symptoms are often similar to other conditions, such as obesity and lymphedema. Additionally, the cause of lipedema is still unknown, although it is believed to be a genetic disorder triggered by hormonal changes.
The most common symptom of lipedema is swelling of the legs and buttocks, and oftentimes the arms and abdomen. This swelling is usually symmetrical and occurs mainly in the lower parts of the body. It can also cause a feeling of tightness in the affected area, as well as aching, burning, and tenderness. The skin in the affected area may also appear dimpled, and the affected person may experience difficulty walking and standing for long periods.
In addition to physical symptoms, people with lipedema may also experience psychological symptoms such as low self-esteem and depression.
Lipedema can be difficult to diagnose because its symptoms are often similar to other conditions, such as obesity and lymphedema. To diagnose lipedema, your doctor will do a physical exam and ask about your medical history. They may also order tests, such as an ultrasound or MRI, to get a better look at the affected area.
Once lipedema is diagnosed, treatment may include lifestyle changes, such as diet and exercise, to reduce swelling and pain. Compression garments can also be used to help reduce swelling. In more severe cases, liposuction or liposculpture may be recommended to remove the excess fat.
A lot of women with lipedema have back pain because the “shelf” of weight accumulated on the lower back distorts the spine. The distortion from the fat lobule over the shelf will be sore if patients are on their feet or sitting for long periods. Many patients have chronic lower back pain without any relief because the constant existence of heavy lipedema tissue causes it.
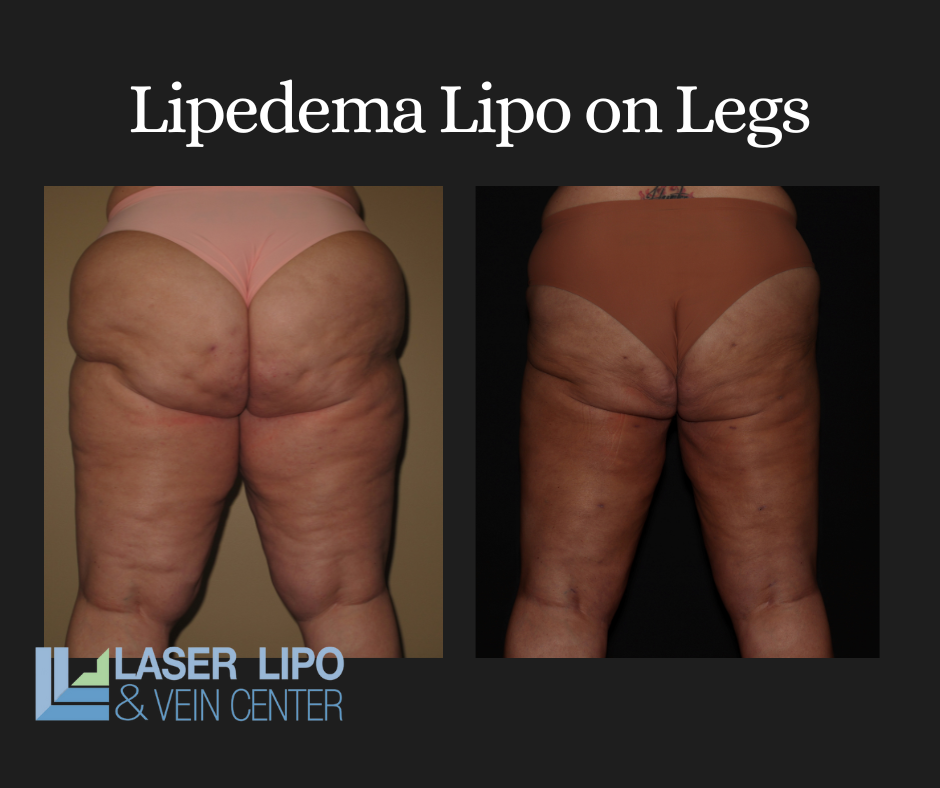

Within a day or two after the tissue removal, patients report experiencing relief never experienced before. Unlike a pulled back muscle or a pinched nerve, surgery and the removal of this area’s fatty tissue and fluid is the only way to get relief.
Lipedema surgery is a life-changing solution for those suffering from lipedema of all types and stages, and especially with chronic secondary issues like back pain. This surgery involves the removal of excess fat from the affected area through liposuction or liposculpture. This surgery can help reduce the swelling, discomfort, and pain associated with lipedema. It can also improve mobility, reduce the risk of infection, and improve self-esteem.
There are many benefits to undergoing lipedema surgery. It can help reduce the swelling and pain associated with lipedema and improve mobility. It can also reduce the risk of orthopedic complications and improve self-esteem. Additionally, lipedema surgery can help reduce the risk of developing lymphedema, which can be a severe complication of lipedema. For patients with back pain, the surgery can provide almost immediate relief and allow them to have the ability for daily tasks once again once impossible – as simple as getting a good night’s rest, or the ability to perform accessible exercises more comfortably, like yoga and deep, restorative stretches.
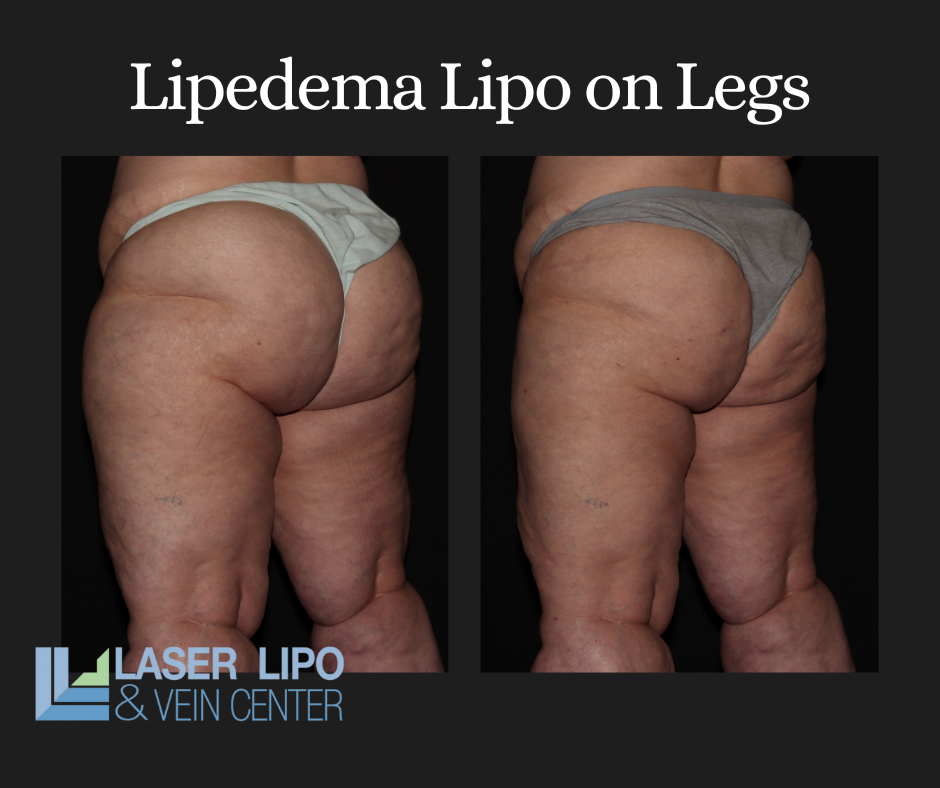

Lipedema surgery can be an effective treatment for those who have experienced significant weight loss. After weight loss, the skin in the affected area may be loose and saggy. Lipedema surgery can help to tighten and firm the skin and reduce the swelling and pain associated with lipedema.
Recovery from lipedema surgery can take several weeks. During this time, it is important to rest and avoid strenuous activities. Your doctor may also recommend compression garments to help reduce swelling and improve comfort.
Lipedema surgery is a life-changing solution for those suffering from lipedema. It can reduce the swelling and pain associated with lipedema and improve mobility. It can also reduce the risk of infection and improve self-esteem. If you are suffering from lipedema and are looking for a solution, contact Dr. Wright and Laser Lipo and Vein Center for help with lipedema and back pain.


Have you ever wondered why some women have no issues maintaining their weight, despite your constant struggle to lose weight no matter what you do? Have you ever heard of Lipedema Legs? If you’re a woman and have noticed weight gain in your lower body that you can’t seem to control, you may have lipedema. Lipedema is a chronic and progressive medical condition that affects the limbs (and sometimes the abdomen, too!) of women. In this blog, we’ll be exploring the causes, symptoms, and treatment options for lipedema legs.
Lipedema is a medical condition that affects many women worldwide. The condition is also known as Lipoedema. It is a disorder that causes fat to accumulate in the legs, hips, buttocks, arms, and/or abdomen of many women. Fat accumulation occurs in the form of nodules and can cause pain, inflammation, and swelling. It is estimated that 11% of women in the United States suffer from lipedema, and most are unaware of their condition.
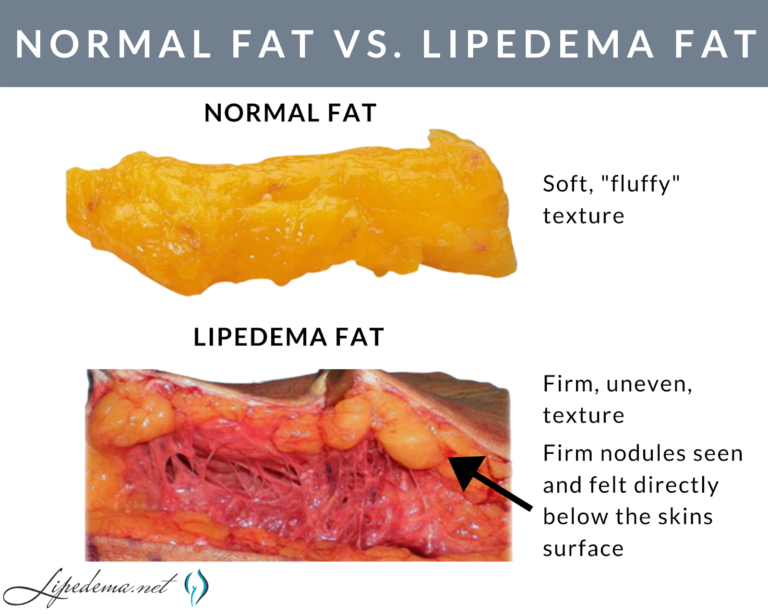

Lipedema is believed to be linked to genetics and hormones. Research suggests that hormones such as estrogen may play a role in the development of lipedema. It is also thought that lipedema has a vital hereditary component, meaning if your mother or grandmother had lipedema, you might be more likely to develop the condition. The symptoms of lipedema legs vary from person to person. The most common symptom is swollen legs, especially in the lower legs. Other symptoms include pain, tightness, and discomfort. In some cases, lipedema can cause pain, numbness, and tingling in the legs. The leg fat can also be easily bruised and is often resistant to diet and exercise.
Lipedema legs can cause a wide range of symptoms, including swelling, pain, and tightness in the legs. The leg fat can also be easily bruised and is often resistant to diet and exercise. In some cases, lipedema can cause numbness and itchiness or tingle in the legs. In addition, leg fat can cause an uneven weight distribution, resulting in pain and discomfort.
The symptoms of lipedema can vary from person to person. Some people may experience little to no symptoms, while others may experience more severe symptoms. The severity of the symptoms can also vary over time.
The diagnosis of lipedema legs is based on a physical examination and a review of the patient’s medical history. The doctor will look for signs of fat accumulation in the legs, hips, and buttocks. They may also check for signs of inflammation and swelling. The doctor may also perform a lipedema test, which involves measuring the circumference of the legs, hips, and buttocks. This test can help determine if the patient has an accumulation of fat in the affected areas. In addition, the doctor may perform a stemmer sign test.

The stemmer sign is a test used to diagnose lipedema. The test involves pressing the thumb against the skin of the affected area. If the skin does not indent, this is a sign of lipedema. This test is used to differentiate between lipedema and other causes of swollen legs, such as lymphedema. The stemmer sign test can also help determine the severity of the lipedema. In mild cases, the skin may indent slightly, while in more severe cases, the skin may not indent at all. This can help the doctor determine the best course of treatment for the patient.
Once the diagnosis of lipedema legs has been made, the doctor will recommend a treatment plan. The treatment plan will vary depending on the severity of the condition. In mild cases, the doctor may recommend lifestyle changes such as diet and exercise focused on decreasing inflammation triggers. Medical-grade compression help reduce the inflammation is lipedema tissue in the legs. In more severe cases, the doctor may recommend medication or surgery. Medication and surgery are typically used to reduce the swelling and inflammation associated with lipedema. Medication can help reduce the number of fat cells in the affected area and can also help reduce swelling and inflammation. Surgery can help remove fat cells from the affected area and can also help reduce swelling and inflammation.
If you think you may have lipedema, you must see a doctor. The doctor will perform a physical examination and review your medical history. They may also perform a lipedema test and a stemmer sign test. Once the diagnosis has been made, the doctor will recommend a treatment plan. Treatment may include lifestyle changes, medication, and surgery.
Lipedema legs can be a difficult condition to live with, but with the right treatment, it is possible to manage the disease. With the right treatment, you can live a healthier and more active life.


One of Dr. Wright’s newer patients, Crystal, was diagnosed with Lipedema for the first time just 3 months ago, and she’s already feeling the joy and relief that comes with an official Lipedema diagnosis.
“I felt a sense of relief and joy come over me instantly,” she says.
Crystal was diagnosed by Dr. Wright with Stage 3, Type 3, and 4 Lipo-Lymphedema. Over the next 90 days post-diagnosis, she’s undergone two Lipedema surgeries and overcome a lifetime of challenges when it came to “her relationship with gravity”, as she calls it. She lost just over 70 pounds after the two surgeries and is relieved to be on a path of healing.


Lipedema is a fat disorder, mainly affecting women, that causes an enlargement of both legs due to deposits of fat under the skin. It’s characterized as a “progressive disorder,” meaning it generally gets worse over time. In severe and more progressive cases, the trunk and upper body may also be affected, including the arms and upper back, and it’s often misdiagnosed and incorrectly treated as general obesity.
Nearly 17 million women in the U.S. and nearly 370 million women across the globe suffer from Lipedema. What is regularly associated with unruly weight gain in its initial stages can quickly spiral out of control if left undiagnosed. Often striking in a woman’s mid-20s, Lipedema is a disease that leads to the excessive buildup of fat cells primarily in the arms and legs. Going far beyond the appearance of extra pounds, those who suffer from Lipedema often present with pockets of fat on the limbs that appear disproportionate in comparison to the rest of the body.
Women suffering from this disease often report the association with lipedema pain symptoms that trigger difficulties dealing with everyday life activities. Excessive swelling often comes with pain, numbness, and bruising. In its advanced stages, Lipedema can impact mobility and provokes vascular and lymphatic swelling which can lead to further medical complications.

Lipedema is often misdiagnosed as standard obesity, leaving patients to deal with an endless cycle of disappointment and ongoing, painful lipedema symptoms. As they continue, their weight refuses to fall off. Unfortunately, Lipedema does not respond to a simple calorie restriction or increased exercise and ultimately requires surgical intervention in order to alleviate the appearance and pain of symptoms.


Patients often report that the road to their initial Lipedema diagnosis is an uphill battle. Women with Lipedema are typically diagnosed by their primary care provider with traditional obesity, and all treatment methods follow this diagnosis.
Unfortunately, as any Lipedema specialist will tell you, this treatment proves ineffective, and leaves women with Lipedema without answers, without a solution, and with continued pain and continued frustration as their, Lipedema continues to progress. Liposuction performed on the affected limbs is one of the most effective forms of treatment. Removing fat deposits that are diseased not only helps reduce swelling of the limbs but alleviates the pain that holds patients back from everyday activities. But before women with Lipedema and even consider these procedures and treatment options, they must first find a doctor who is an expert in this field and start with a proper diagnosis of the disease.
Just like Crystal, many women search for answers for years before getting an official diagnosis and validation for their struggles. “My body really needed this healing,” Crystal says. “I needed answers and I was craving [an] explanation why my body was fighting me.” While she contributes 15 pounds lost directly to her surgeries, she says she’s done the non-surgical work to get rid of additional lipedema swelling and fluid alongside surgery. She says she monitors what she eats and when, and eliminated a few types of foods that directly increase swelling, helping her lose more than 50 pounds on her own, and improving the outcomes of both her surgeries tenfold.
She encourages other women who think they may have Lipedema to contact Dr. Wright and his team to get the same help she’s received. “If you have lipedema or lipo lymphedema like I do, go easy on yourself,” she says. “There isn’t anything you could have done to prevent it, but I’m living proof there are things you can do to live better and have a higher quality of life.”
The story is almost always the same, and we hear it all the time; women are living in pain for the majority of their lives, begging for medical explanations and solutions, and are coming up empty. These women spend years – sometimes decades – struggling with uncontrollable and disproportional weight, deep bruising and tender skin from the lightest of touches, and have constant swelling. Their weight gain is typically in their limbs or “trunk” and widely does not affect their feet, hands, or upper body from the waist up. These symptoms progress, cause more pain, and often get to the point that women are unable to walk upstairs, take a brisk walk, or even sit for long periods of time without feeling intense pain and discomfort.
The consistent diagnosis from their primary care doctors centers around their weight, and are diagnosed for general obesity, and prescribed treatments that range from diet and exercise to more extreme surgeries to curb appetites and encourage weight loss. Unfortunately, for those who have Lipedema, these treatments will turn up useless and ineffective, yet their doctors assume the issue is from the patient’s lack of dedication to the prescribed program, rather than the misdiagnosis of the disease known as Lipedema.


Despite affecting an estimated 11% of women around the world, Lipedema is not yet widely known. Fat cells, (also referred to as adipose tissue) provide the human body with both cushioning and insulation. Lipedema affects the accumulation of these fat cells in the body, resulting in bulging, irregular fat in the affected areas. The legs are the most commonly affected area, but sometimes spreading occurs in the torso, and in many cases, excessive clustering of fat cells is noticed in the arms as well. Regardless of the affected area, the symptoms are equally debilitating, and unfortunately, these fat cells are equally resistant to both diet and exercise programs.
Unlike Lymphedema or general obesity, Lipedema has a tendency to affect both limbs equally and generally becomes more apparent over the course of time. Lipedema’s progressive nature makes getting a proper diagnosis and treatment imperative and extremely time-sensitive – as the disorder progresses so does the pain, immobility, and discomfort.
In addition to the characteristic disproportionate fat accumulation, there are specific physical signs and symptoms of Lipedema. Do any of the following Lipedema symptoms sound like something you regularly experience?
Lipedema Symptoms Checklist:
☑Tender skin that is sensitive to the touch, feels pressure when walking or climbing stairs, crossing your legs, or sitting for long periods of time.
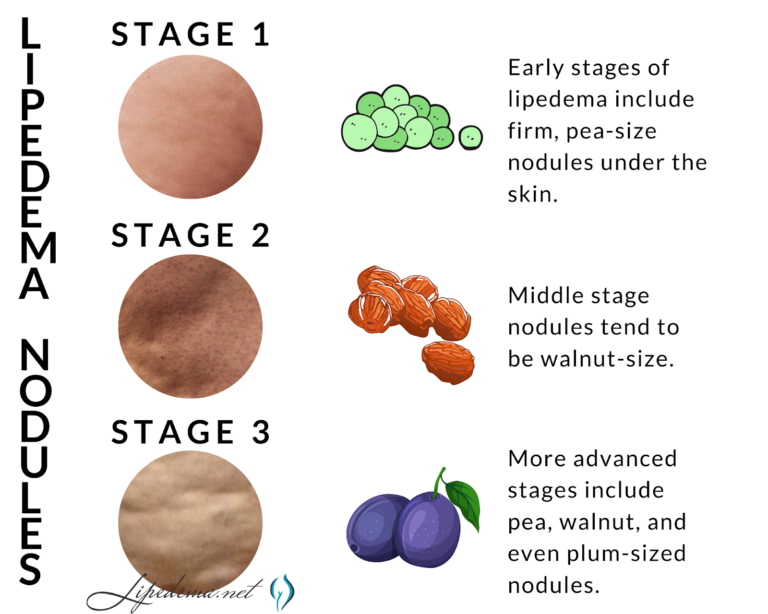
☑Skin’s surface feels nodular and firm, like beans in a bean bag or rubber balls.
☑Skin’s surface is uneven, with large bulges and valleys up and down. Areas that were traditionally thought of as cellulite are much more dramatic and bulging.
☑Skin’s temperature is relatively cool.
☑Legs feel heavy and tired.
☑Swelling in the affected area (legs, arms), worsening during the day, and better at night after you’re able to elevate your limbs (such as laying in bed).
☑Easy bruising.
☑Visible veins.
☑Disproportionate fat accumulation, not affected by calorie restriction. Think extreme “pear-shaped” body.
☑Feet and hands are unaffected by weight gain or swelling. As a result, there’s often a “cuff” at the ankles or wrists.
Overall, Lipedema appears in a series of three stages. Do any of these sounds like you?
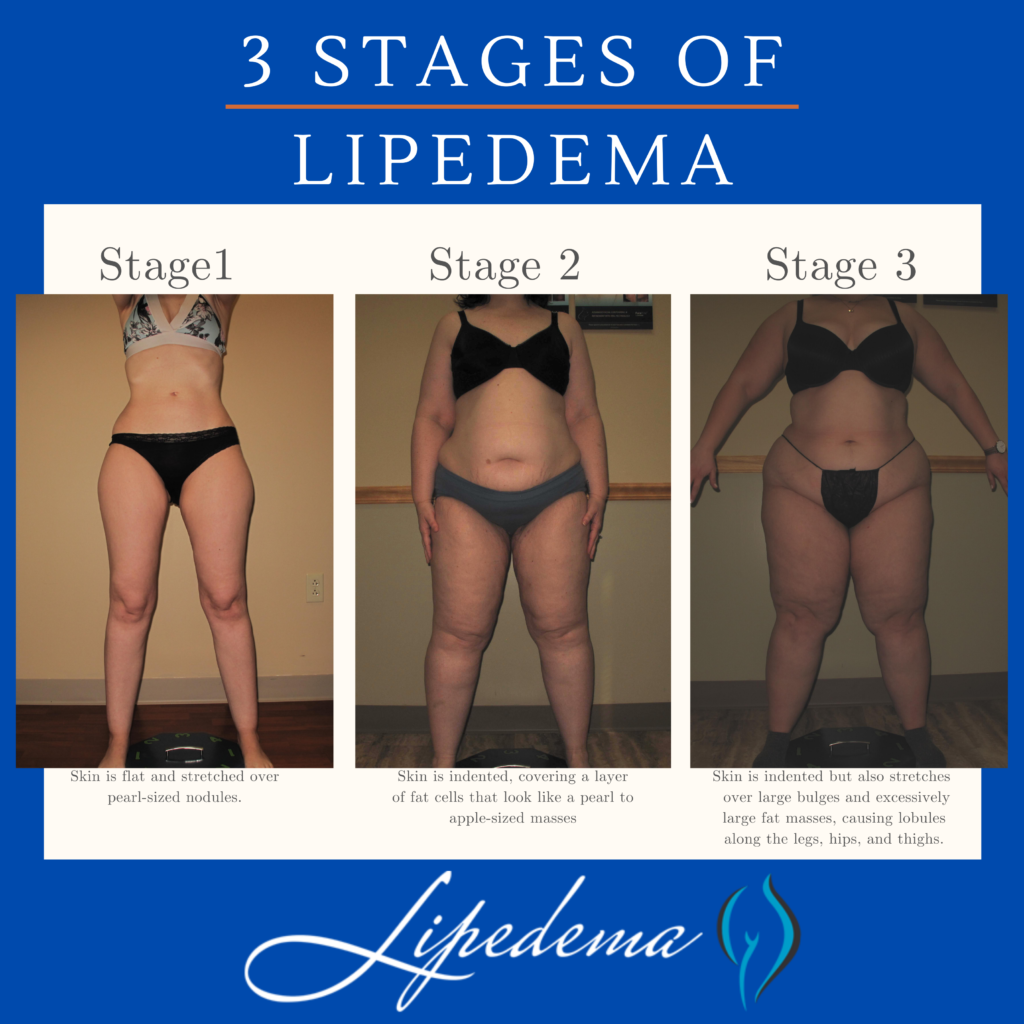

If one of these stages sounds like you, and you checked off multiple items on the list above, you may have Lipedema, but it’s impossible to say for sure. The only way to know for sure is to get a proper Lipedema diagnosis, which in itself is an important process.
The diagnosis of Lipedema is made based on a clinical evaluation from a physician with specific knowledge and experience of the disease in combination with supporting tests that rule out other diagnoses. For this reason, it’s no surprise that Lipedema is a poorly recognized and under-appreciated disease in the United States – it takes an expert to recognize it, and finding an expert is tough if you’ve just learned about it yourself! The recognition of characteristic features of Lipedema and the elimination of other conditions that can be confused with Lipedema is the key to the proper diagnosis. We know it can be overwhelming, but knowing as much as possible before speaking with your doctor or seeking out an expert is another tool in your pocket to ensure you receive the care you need. You can read more about related conditions here, but it’s important to know the main points to advocate for yourself.
Below are conditions that can be confused with and can affect people with Lipedema. Because there can be so much overlap in appearance and symptoms, only clinicians with the training and experience to diagnose and treat these conditions can differentiate them. If you’re diagnosed with one of these conditions but you feel strongly that the diagnosis is incorrect, these summaries can help highlight why.
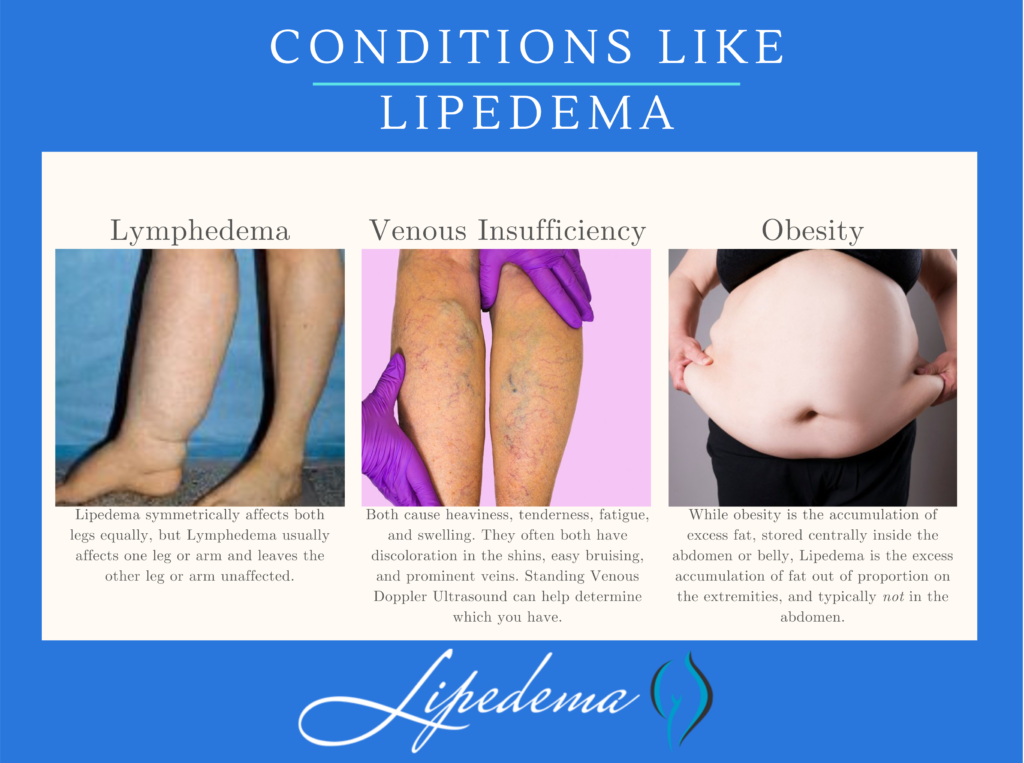
While Lipedema typically does not have to swell in the patient’s feet and hands, Lymphedema will always have swelling in these areas. Lipedema symmetrically affects both legs equally, but Lymphedema usually affects one leg or arm and leaves the other leg or arm unaffected. There may be overlap in these two diseases and treatments can be similar, but some patients only experience Lymphedema after their Lipedema progresses into later stages.
Obesity is much more common than Lipedema, and the most common misdiagnosis for it. While obesity is the accumulation of excess fat, stored centrally inside the abdomen or belly, Lipedema is the excess accumulation of fat out of proportion on the extremities, and typically not in the abdomen or belly. There may be overlap in these two conditions, too. In fact, sometimes obesity develops as a secondary condition due to the mobility problems caused by the Lipedema. So, not only is lipedema often misidentified as just obesity, but obesity can also complicate Lipedema, and be a symptom of it.
The symptoms of Lipedema and venous insufficiency are similar. They both cause heaviness, tenderness, fatigue, and swelling. They often both have discoloration in the shins, easy bruising, and prominent veins. In more advanced cases of venous insufficiency, not only does venous lymphedema develop, but a secondary Veno- Lipo- Lymphedema develops. With the overwhelmed lymph circulation, the ability to clear fatty acids from the affected tissue is compromised and a secondary fat accumulation occurs. In many cases, the best way to differentiate between lipedema and venous insufficiency and veno- lipo-lymphedema is to have a specialized standing venous Doppler ultrasound to check for venous reflux.

Now that you’ve reviewed the signs and symptoms of Lipedema, determined that you identify with at least some of them, and you’ve familiarized yourself with other commonly related diagnoses, it’s time for the final step – finding a Lipedema specialist and getting tested! Each Lipedema doctor will have their own preferred method of diagnosing their patients and typically will include a physical exam, patient questionnaires, and then additional testing and ultrasounds to further support the physical exam.
Below are the different tests you may experience during this time, and it’s important to keep them in mind as you select your doctor. Moving forward, thoroughness will be your best friend; we highly recommend “interviewing” different Lipedema experts to find someone you trust, someone who can provide at least some of these diagnostic tests, and someone who is well versed in treatment options.
The Stemmer’s Sign is the inability to pinch the skin between the toes or fingers. As mentioned in our last section, Lipedema in advanced stages can be complicated by secondary Lymphedema and may have a stemmer’s sign. This test can help Lipedema experts determine if this is the case for you.
A Venous Doppler Ultrasound is a very useful test for the diagnosis of Lipedema. Lipedema has many similarities to venous insufficiency (as explained above), so this can help rule out or confirm venous insufficiency. The Venous Doppler Ultrasound can readily detect venous insufficiency if done properly and by having the patient stand while completing it. Unfortunately, most hospital vascular labs complete Venous Doppler Ultrasounds with the patient lying down, While this is the typical way to find Deep Vein Thrombosis (DVT), it is definitely not a successful method to detect venous insufficiency. A standing venous Doppler ultrasound is a painless, non-invasive, and inexpensive test that provides a lot of useful information about venous circulation. The Doppler ultrasound not only helps determine the presence of underlying venous problems, but it also gives critical information for managing Lipedema. If venous insufficiency is present, it is important that treatment is given as the resulting increased venous pressures can greatly aggravate Lipedema.
This is generally only used in complicated cases, where clinical diagnosis is not clear. This is a nuclear scan that assesses the lymph system. It may come back as normal in patients with Lipedema and may show the characteristic “corkscrew” changes with Lymphedema. In most cases of Lymphedema, lymphoscintigraphy shows delayed uptake. So lymphoscintigraphy can be very helpful to determine if and how significant a role lymphedema is playing in an individual’s symptoms, especially when there are widespread issues of swelling in the body.
First – congratulations! We know the road to diagnosis is emotionally draining, physically painful, and it can feel lonely and discouraging. The time and research it takes to make it to this point are huge, and you should be proud of yourself and the courage it takes to be your own advocate. Our hope for all women with Lipedema, whether they are our patients or not, is that we can provide valuable tools and knowledge so that more women can make it to this point and take the next step in living a more mobile, healthy, and enjoyable life.
After going through the diagnosis process and receiving a positive Lipedema diagnosis, most patients are relieved, overjoyed, and validated by their endless search. After years of living with the private struggle and knowledge that “something just isn’t right” in their body, putting a name to the issues is a huge win. And after an official diagnosis, there are many different treatment paths available to you! A treatment plan should be discussed and developed between you and your Lipedema doctor, but you can read more about non-surgical and surgical options that we recommend to our patients. While these will always depend on specific cases and patient needs, it can give you an idea of what options may be available to you. Good luck!
Lipedema continues to be a poorly identified condition where diagnoses are often avoided by US physicians. Identifying lipedema involves a clinical evaluation from a medical physician with expert knowledge regarding this condition. Two factors that are critical in finding a proper lipedema diagnosis include identifying an abnormal fat deposition in impacted areas and identifying symptoms of lipedema.
Far too often Lipedema is misdiagnosed as obesity. The abnormal fat deposition of lipedema is very different from obesity. Individuals with lipedema typically accumulate disproportionate fat in soft tissue just below the skin on the arm and legs. Individuals with obesity typically see a proportional increase of fat issue around the body but it is more concentrated inside the abdomen, called visceral fat. Individuals with lipedema will instead see a much greater fat accumulation be around extremities and not the abdomen which is described as disproportionate when compared to the rest of the body.
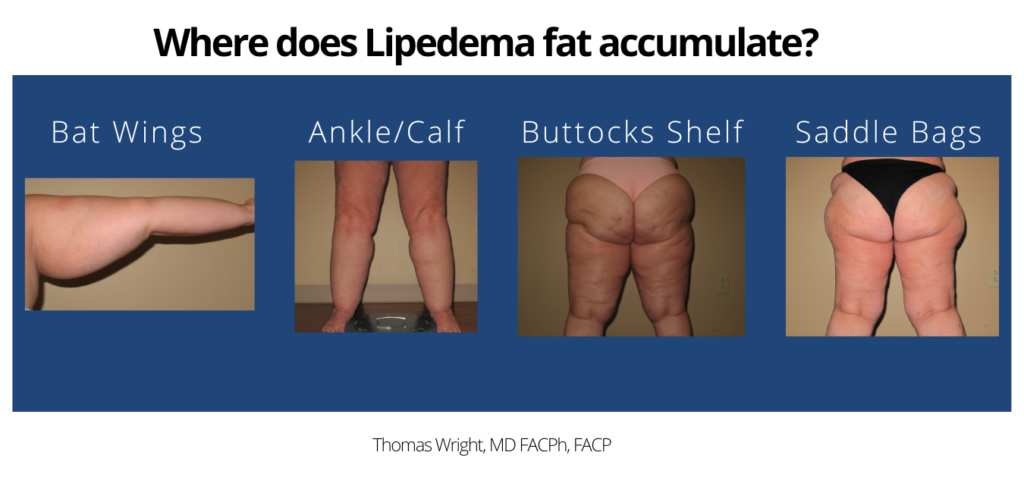
Lipedema can be identified with five different types of the condition depending on where the fat tissue is found predominantly. Type I identifies lipedema with fat pockets around the buttocks. Type II identifies lipedema with fat around the hips and thighs in addition to the buttocks. Type III identifies fat tissue around the calves, ankles, and thighs. Type IV identifies lipedema with pockets of fat tissue on the arms while Type V is lipedema with fat tissue found exclusively on the calves and ankles.
Where does lipedema fat accumulate? Find out here.
It helps to properly identify lipedema by recognizing many of its common symptoms. Individuals who have been properly diagnoses often have tender skin that is sensitive to walking and pressure. Limbs affected by lipedema appear to be “fluffy” and have a rubbery feel to them. The skin tissue will eventually harden and feel like beans in a bag. Skin tissue will also lose elasticity and become uneven. The overall temperature of the skin will cool. Your legs will begin to feel heavy and lead to overall fatigue. Individuals with a newer development of lipedema will see that swelling will be frequent during the day and subside at night. Individuals who have been dealing with lipedema for years will notice that the swelling will progress at later stages. Finally, individuals with lipedema will also notice visible veins under the skin on impacted limbs and will bruise easily.
Properly identifying symptoms of lipedema and observing abnormal fat distribution will help with diagnosing this condition. Physicians now use tests to help with their diagnoses such as venous Doppler ultrasound and lymphoscintigraphy. Additional research will help with properly identifying lipedema from obesity and other fat-related conditions. Contact us for your proper lipedema diagnosis.
When most think of lipedema, they think of the changes in size the body will go through as the disproportionate fat tissue accumulates. This fat tissue is disproportionate, as it typically builds up most around the lower extremities such as the hips and thighs. This change can hurt the way you think you look and harm your social relationships. However, lipedema can do much more than just harm your self-confidence. Lipedema causes arthritic symptoms similar to that of degenerative joint disease. This condition disables most individuals, causing them mobility issues.
Mobility causes stem from the fat tissue on the inner thigh puts pressure around the medial knee compartment. This increase of pressure will lead to acceleration knee joint degeneration that could require an eventual knee replacement. However, the buildup of pressure also applies further down the leg as well increased pressure on inner half of the leg lead to flattening of the plantar, foot, arch. The distal back of thigh and the back calf can also interfere with mobility even further by restricting the flexion (bending) of the knee.
One way that degenerative joint disease can impact your mobility is through causing a restricted range of motion. The range of motion in one’s legs is identified through a term called flexion, which is measured in degrees. An individual without lipedema typically has a full range of motion of up to 140 degrees. Individuals with lipedema can have a flexion reduced to only 90 degrees, considerably less than those without lipedema. The fat tissue around the knees can make full motion virtually impossible. This mobility issues from lipedema will persist even when a knee replacement is done, and you will not find much success without first dealing with the fat tissue.
Before a knee replacement can be completed, it is recommended that the fat tissue in and around the knee be removed with liposuction. Current procedures are now minimally invasive to ensure success and comfort of the patient. Once the fat tissue has been removed, the success of a knee replacement is exponentially increased. Reducing this fat tissue will also reduce the pressure on your knee and surrounding leg, leading to greater activities of daily living.
As you can see, lipedema impacts more just self-image; it can do irreparable damage to your knees and surrounding leg tissue. Seek out the treatment you need with lipedema specialists such as Dr. Wright. Your lipedema treatment plan can help you achieve greater mobility and reduce the impact lipedema has on your daily life. Contact us today!
As you may have noticed, the healthcare industry has been turned upside down by the sudden onset of COVID-19. Several businesses that are deemed non-essential have temporarily closed their doors until further notice, while others are available only for emergency or essential procedures. This can include many places where you can seek relief for your lipedema symptoms. Fortunately, there a few at-home exercises and measures you can take to manage your symptoms of lipedema.
There a several different low impact exercises you can try at home to manage your lipedema symptoms. These exercises include shoulder shrugs, neck rotations, hip abductions, ankle pumps, and bent knee fall outs. The exercises are designed to help stretch out your lymphatic system allowing lymph fluid to flow easier.
General workouts designed to fight off lipedema symptoms are different than the exercises described above. One of the best yet hardest ways to fight off lipedema symptoms is to follow a workout regimen at home. Healthy exercise helps us develop muscle tissue and promote lymphatic circulation. Most of these workouts are low impact and will not be stressful on your joints. These workouts include swimming and water exercises, walking with supportive footwear, elliptical machines and stationary bike rides. Ellipticals and stationary bikes even allow you to change the resistance so you can find the perfect balance of cardio and strength building.
One of the most common lipedema symptoms patients will experience is swelling. Not only does swelling look unattractive but it can also be painful. One conservative treatment option you can do from home is wearing compression sleeves or garments. They can reduce your swelling and help the flow of lymphatic fluids in your affected limbs. These garments are recommended to be worn all day, so it is important to find your correct size.
By maintaining a nutritious diet, you can help reduce inflammation, another common symptom of lipedema. Your diet should include plenty of fatty acids that can help reduce your inflammation and overall swelling. Foods you will want to stay away from include processed packaged foods, wheat and gluten products, refined carbohydrates, dairy products, and food that is high in trans-fat.
While some healthcare offices may be closed, several physicians, including our own Dr. Wright, are introducing video consultation to better support their clients. Make sure to stay in contact with your physician and seek out their advice during this time!