In celebration of Lipedema Awareness month back in June, Dr. Wright and Dr. Herbst updated the world on the latest insights and understandings on Lipedema vs normal fat. Sponsored by Lipedema UK and Lipedema LIO ITALIA, we’ve summarized the key learnings and helpful information below. Don’t miss updates in the future on our “Lipedema in the News” section, and feel free to watch the full 1.5-hour webinar here.
Lipedema is a fat disorder, mainly affecting women, that causes an enlargement of both legs due to deposits of fat under the skin. It’s characterized as a “progressive disorder,” meaning it generally gets worse over time. Sufferers living with lipedema experience easy bruising and tenderness, pain in the affected areas, and significant disability in daily life. In severe and more progressive cases, the trunk and upper body may also be affected, including the arms and upper back. Little is known about the disorder, and it’s often misdiagnosed and incorrectly treated as general obesity.
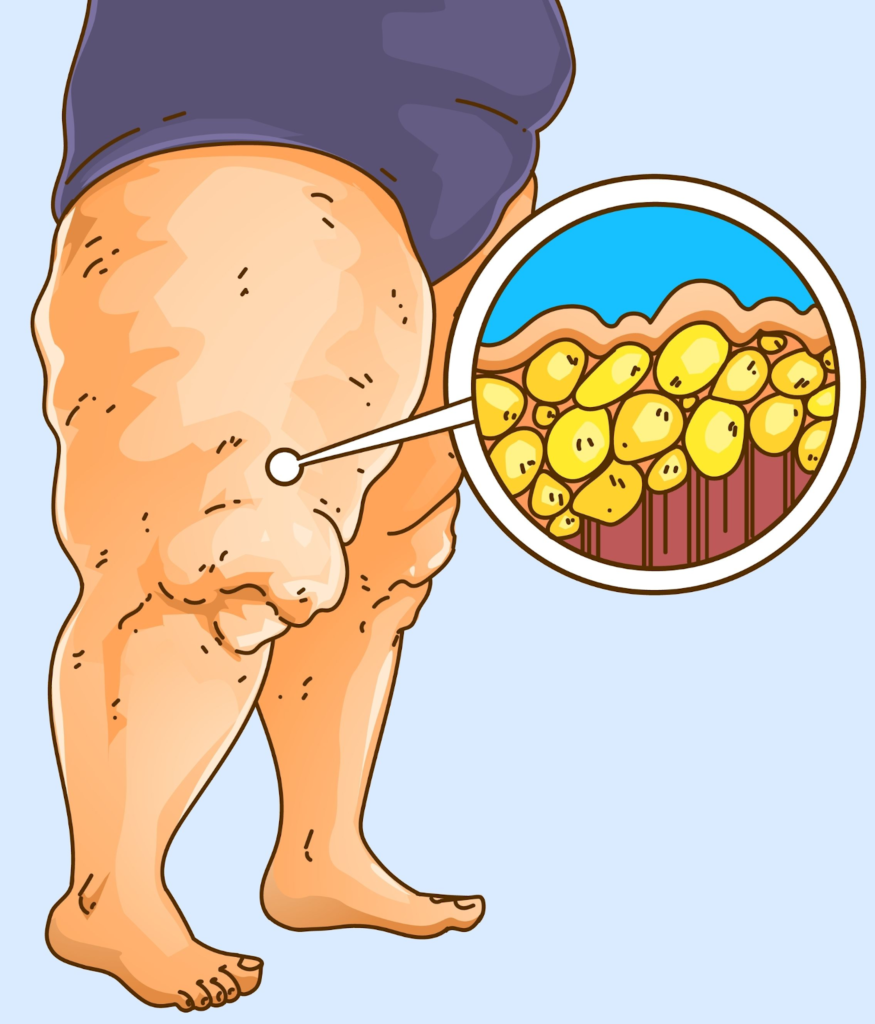

For anyone affected, diet and exercise alone aren’t effective ways to get rid of Lipedema fat; Lipedema fat has proved relatively immune to these lifestyle changes and won’t budge. While women are likely to experience some weight loss with a healthy diet and regular exercise routines, weight loss is usually mostly loss of non-Lipedema fat. In these instances, the painful, stubborn fat remains. This cycle becomes a difficult one to break for those with the disorder: Yo-yo dieting leads to more weight gain. More weight gain leads to increased pain and disability. Increased pain and disability make it more challenging to manage mobility and secondary obesity increases. Lipedema fat also appears to be relatively resistant to bariatric surgery, meaning many women are undergoing dangerous surgeries without experiencing the intended benefit of significant loss of lipedema fat.
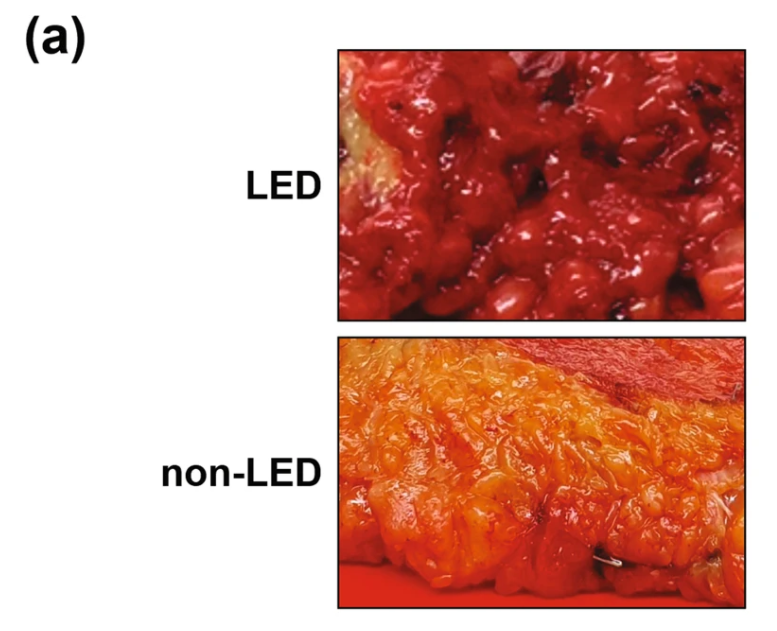

Lipedema adipose fat tissue is different from normal adipose tissue. When looking at this fat tissue in lipedema patients, we find a more fibrous, nodular, tender adipose tissue than in patients without lipedema. The look and feel of lipedema fat tissue can be physically seen when performing lipedema surgery in addition to under a microscope when analyzing the tissue components. It’s clearly a different type of fatty tissue, explaining why lipedema patients experience different side effects and symptoms than those with traditional obesity.
A study published in the International Journal of Obesity in November 2021 (Ishaq et al) highlighted the cellular differences that signaled the differences in lipedema fat than traditional adipose tissue.
The study had the following key findings:
This means that lipedema fat actually causes the body to turn on a different gene than we see in non-lipedema patients. Fat tissue from lipedema was compared to location, gender and age-matched tissue from non-lipedema patients. In the photo below, we see a heatmap gene expression of adipose tissue by Z-score fold-change value: red indicates upregulation and blue indicates downregulation.
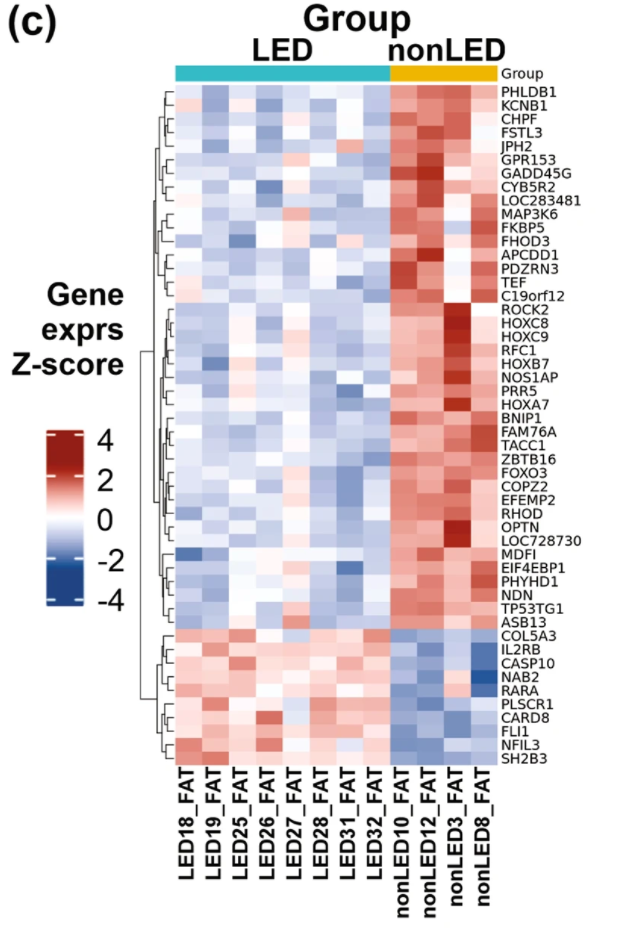

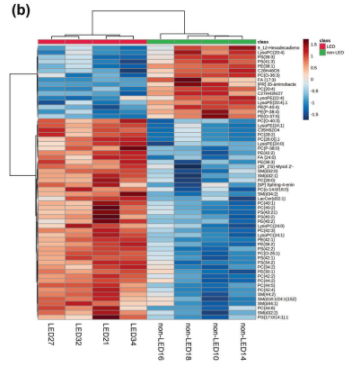
What does this mean? Lipedema fat has a different metabolism, characterized by a differing production of phospholipid production compared to normal fat. Lipedema adipocytes are shown on the left half [Header Bright Red] and non-lipedema adipocytes are shown on the right side of the hierarchal plot of lipid composition [Green Header over columns].

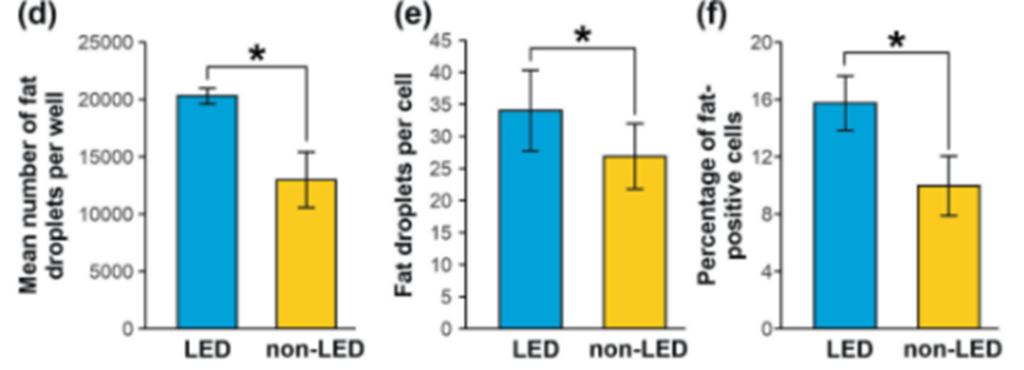
In this study, stem cells [ADSCs] from lipedema fat were compared to stem cells of matched people without lipedema. The stems in lipedema are increased in number.
Note: ADSCs are stem cells. They can continuously divide and renew themselves. The ADSCs stem cells can also become mature fat cells or other types of cells to sustain or grow fat tissue. This means that lipedema fat replicates their cells more than regular fat, increasing the growth of this painful, fibrous fat tissue in lipedema patients!
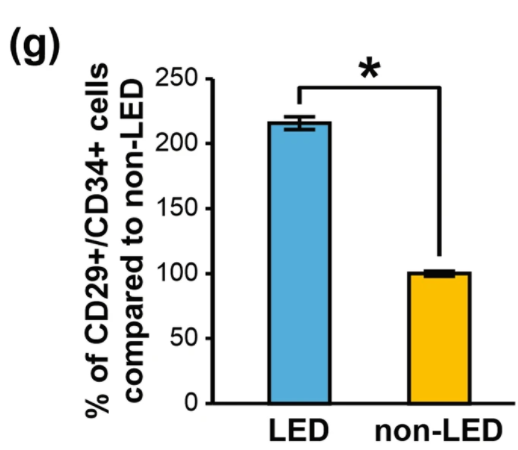

Additionally, Lipedema Stem Cells contain Fat Droplets and have More Fat Droplets per cell than non-lipedema fat cells. The number of fat droplets, percentage of fat-positive cells, and the number of fat droplets per cell were significantly increased in lipedema adipocytes compared to controls. Lipedema fat cells had more fat in them, and the presence of fat droplets in stem cells (ASCDs) indicates maturation toward an adipocyte.

Cell-cycle genes involved in regulating cell growth and proliferation are dysregulated in lipedema ADSCs and may contribute to the increased adipocyte number, and maldistribution and accumulation of dystrophic fat in lipedema. Because of the lack of regulation, lipedema cells again are able to replicate and grow at a higher speed and frequency than non-lipedema fat.
For example, Bub1, which is one of the cell cycle genes, is turned on more or upregulated in lipedema.
First, and most validating for people with lipedema, these findings prove that lipedema fat and normal fat are not the same. Adipocytes and stem cells from individuals with lipedema are structurally different and behave differently from cells of normal fat tissue. Second, diet and general nutrition do not affect lipedema fat in the same way it does for non-lipedema fat. Given the same nutritional support, lipedema-derived stem cells proliferated compared to normal fat-derived stem cells. And third, the faster growth of lipedema fat compared to non-lipedema fat can be explained at a cellular level. The different cell biology of the lipedema cells that leads to hyperproliferation of fat tissue may explain disproportionate growth compared to other adipose tissue.
While these lipedema vs normal fat findings are exciting for lipedema providers, and even more validating for patients seeking insights and treatment options, one question still remains: Is the biology of lipedema fat different because of genetic differences or is the difference in the fat cell biology of lipedema a product of an altered environment?
Even with all the challenges presented by lipedema, there are those who you can trust. Dr. Wright continues to strive for better education, research, and coverage for the lipedema community. Do not let these challenges bring you down even further; let Dr. Wright and his expert team help you to reduce the symptoms of lipedema and live your life fully! Dr. Wright can help find the right procedure to help manage your lipedema symptoms. Don’t let lipedema take over your life; contact us today!