June is Lipedema Awareness Month, a time dedicated to raising awareness, providing resources, sharing knowledge, and advocating for equitable healthcare for patients with this complicated, misunderstood, and often misdiagnosed disease. This article will explore the history of lipedema, its symptoms, stages, diagnosis, treatment options, and the importance of research and awareness campaigns. By understanding the key aspects of lipedema and its management, we can help support those affected by the condition and contribute to a more informed and inclusive healthcare system.
What is Lipedema?
Lipedema is a fat disorder that mainly affects women and causes enlargement of both legs due to fat deposits under the skin. It’s characterized as a “progressive disorder,” meaning it worsens over time. In severe and more progressive cases, the trunk and upper body may also be affected, including the arms and upper back, and it’s often misdiagnosed and incorrectly treated as general obesity.
Lipedema is a disease that leads to the excessive buildup of fat cells, primarily in the arms and legs. Going far beyond the appearance of extra pounds, those who suffer from Lipedema often have large pockets of fat on their limbs that appear disproportionate compared to the rest of the body. Medical professionals often misdiagnose and dismiss lipedema as simple obesity, leaving affected women with an endless cycle of disappointment, frustration, and pain. Lipedema does not respond to a diet and exercise routine, yo-yo dieting, or juice cleanses.
Women suffering from Lipedema often report the disease associated with painful symptoms that trigger difficulties in dealing with everyday activities. Excessive swelling often comes with pain, numbness, and bruising. In its advanced stages, Lipedema can impact mobility and provoke vascular and lymphatic swelling, leading to further medical complications.
Symptoms of Lipedema
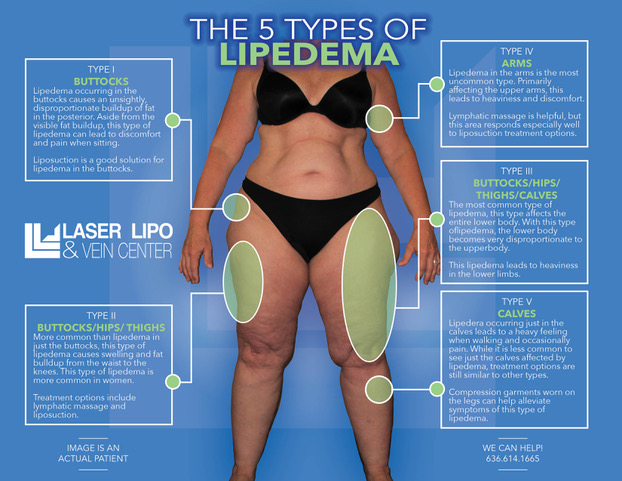
Lipedema is characterized by an abnormal accumulation of fat cells in the body, resulting in bulging, irregular fat in the affected areas. The legs are the most commonly affected, but the condition can also spread to the torso and arms. Symptoms of lipedema can be debilitating, and the fat cells associated with the condition are resistant to both diet and exercise programs.
Some common symptoms of lipedema include:
- Disproportionate fat accumulation in the extremities, often with a significant difference between the upper and lower body
- Pain, tenderness, and swelling in the affected areas
- Easy bruising and sensitivity to touch
- A feeling of heaviness or fatigue in the limbs
- Limited mobility and decreased range of motion
- Skin appears stretched and shiny over the fat deposits
- Fat deposits that are soft and doughy to the touch
Stages of Lipedema
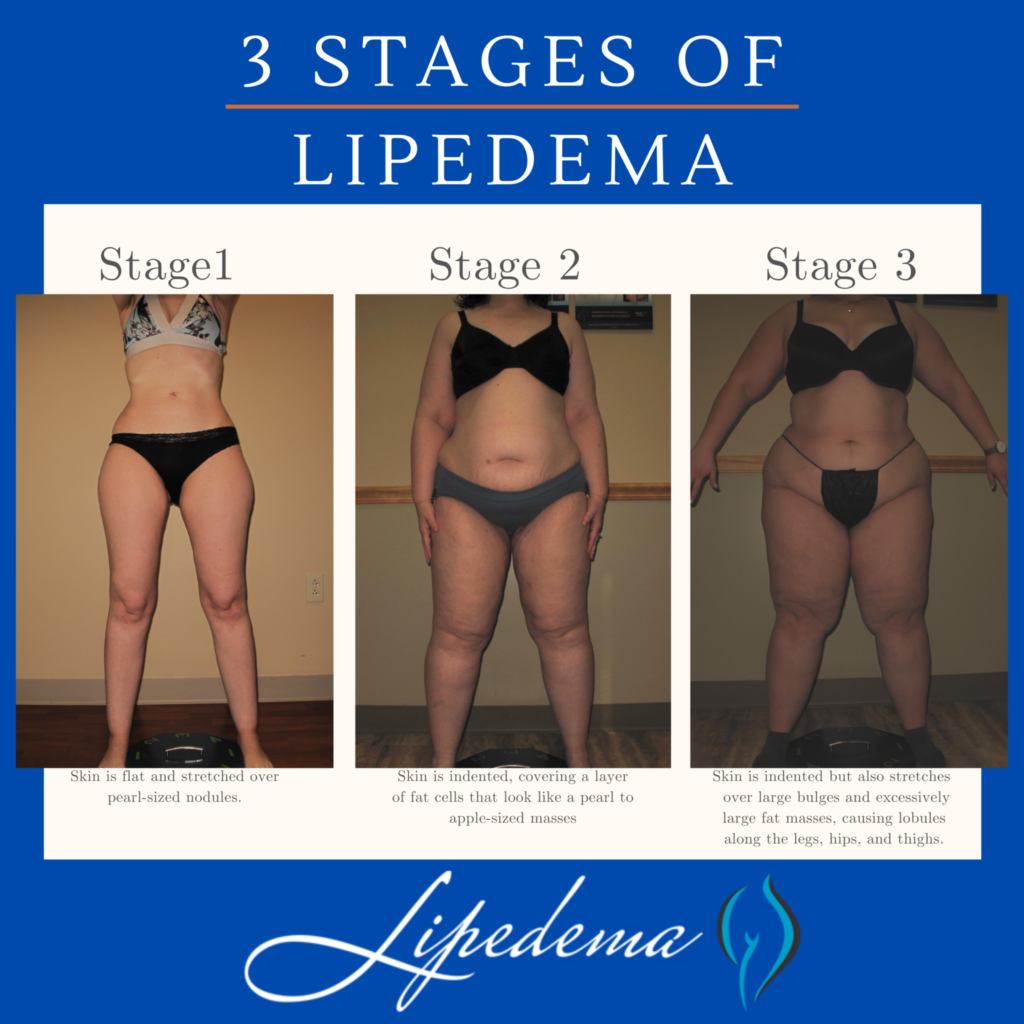
Lipedema progresses through three distinct stages, each with its own set of characteristics:
- Stage 1: The patient’s skin is flat and stretched over small, pearl-sized fat nodules.
- Stage 2: The patient’s skin is indented, covering a layer of fat cells that resemble pearl to apple-sized masses.
- Stage 3: Skin is indented, sometimes with much larger bulges, and covers pearl-sized nodules in combination with excessively large fat masses. This stage may cause lobules along the legs, hips, and thighs and can extend to the torso or upper arms.
Conditions Often Confused with Lipedema
Several conditions can present similar symptoms to lipedema, making accurate diagnosis challenging. These conditions include:
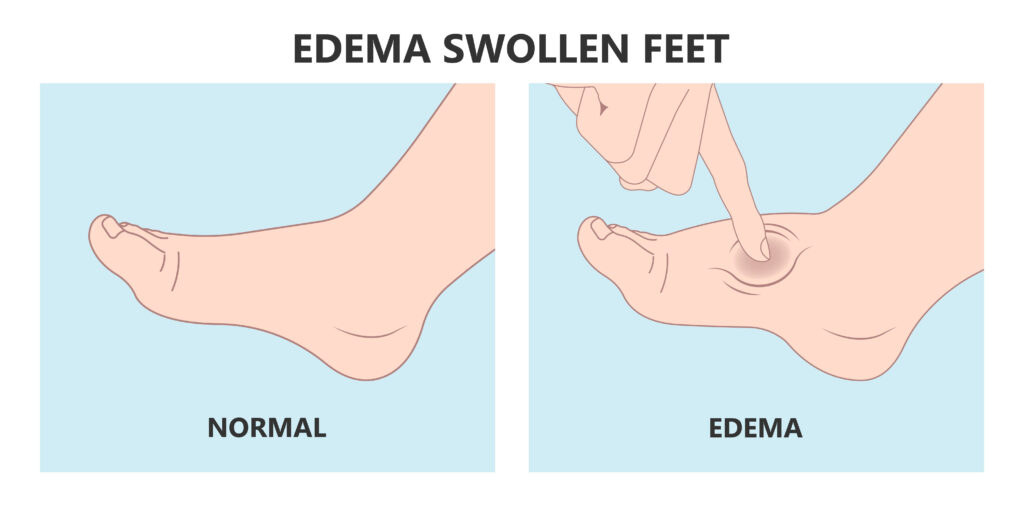
- Lymphedema: A condition characterized by limb swelling due to a compromised lymphatic system. Unlike lipedema, lymphedema typically affects only one limb and often involves swelling in the feet and hands.
- Obesity: A more common condition involving the accumulation of excess fat throughout the body. Obesity is often misdiagnosed as lipedema, though the two conditions can sometimes overlap when obesity develops as a secondary condition due to mobility issues caused by lipedema.
- Venous Insufficiency and Veno-Lipo-Lymphedema: Conditions that affect the veins and lymphatic system, causing symptoms similar to lipedema. Proper diagnosis by trained clinicians is essential to differentiate between these conditions and lipedema.
Diagnosing Lipedema
Obtaining a correct lipedema diagnosis is crucial for effective treatment and management. Diagnosis typically involves a combination of a physical exam, patient questionnaires, and additional testing, such as ultrasounds or Doppler imaging. Some diagnostic tests used to differentiate lipedema from related conditions include:
- Stemmer’s Sign Test: This test examines the ability to pinch the skin between the toes or fingers. A positive Stemmer’s sign indicates the presence of lymphedema, which can sometimes coexist with lipedema, especially in advanced stages.
- Venous Doppler Ultrasound: This non-invasive, painless test assesses venous circulation and can help rule out or confirm venous insufficiency, a condition with symptoms similar to lipedema.
- Lymphoscintigraphy: A nuclear scan used to assess the lymphatic system, typically reserved for complicated cases where a clinical diagnosis is unclear.
Treatment Options for Lipedema
While there is no definitive cure for lipedema, several treatment options can help manage the condition and improve the patient’s quality of life. These treatments may include:
Non-Surgical Treatments
- Conservative therapy: This approach involves the use of compression garments, manual lymphatic drainage (MLD), and other components of complete decongestive therapy (CDT) to manage to swell and improve lymphatic function.
- Nutritional support: A low-carb, ketogenic diet may benefit some lipedema patients, though individual dietary needs should be determined in consultation with a healthcare professional.
- Physical activity: Regular, gentle exercise can help maintain mobility, encourage lymphatic flow, and improve overall health.
Surgical Treatments
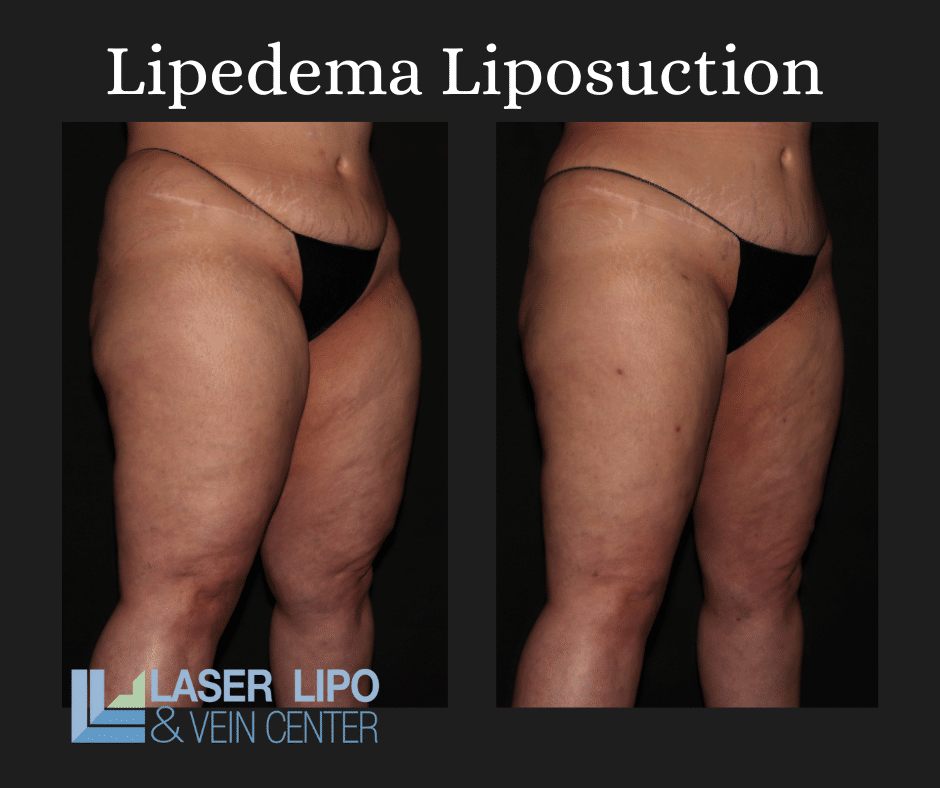
Liposuction: This surgical intervention removes excess fat deposits and may provide long-term relief for some lipedema patients. However, it should be considered in consultation with a qualified healthcare professional and as part of a comprehensive treatment plan.
The Importance of Research and Awareness
Despite being identified over 80 years ago, lipedema remains under-researched and poorly understood. Increased research efforts can lead to improved diagnostic techniques, better treatment options, and a deeper understanding of the condition’s underlying causes. Lipedema Awareness Month serves as an opportunity to raise awareness of the condition, educate healthcare professionals and the public, and support ongoing research initiatives.
How to Get Involved in Lipedema Awareness Month
There are several ways to participate in Lipedema Awareness Month and support patients living with the condition:
- Educate yourself and others about lipedema by sharing resources, such as articles, social media posts, and videos.
- Participate in events, such as webinars, workshops, and support groups, to connect with others affected by lipedema and learn from their experiences.
- Advocate for improved healthcare policies and increased research funding for lipedema.
- Donate to organizations dedicated to lipedema research, education, and support.
In Summary
Lipedema Awareness Month is a crucial time for raising awareness, providing resources, and advocating for patients living with this often misunderstood and misdiagnosed condition. By educating ourselves and others, supporting research efforts, and promoting inclusive healthcare policies, we can contribute to a more informed and compassionate healthcare system for all those affected by lipedema.