Lipedema is characterized by painful and swollen fat which accumulates disproportionately in the subcutaneous tissue. New studies have shown that all stages of lipedema show increased swelling in the lower extremities as measured by Bioimpedance. In a study published this year in the Journal of Lymphatic Research and Biology, Crescenzi, Donahue and Herbst showed that compared to controls all stages of lipedema have increased extracellular water or swelling. (R. Crescenzi, 2019) Further, the study showed that the edema or extracellular water increased with each stage of lipedema. We know that extremity edema or lymphedema is associated with multiple inflammatory processes that are responsible for pain, tenderness and progressive fibrosis of the affected areas. Learn how compression garments can help with lipedema, below.
All the Standard of Care [Dutch (Damstra, 2017), German, and British (Coppel, 2017)] Guidelines for the management of lipedema recommend the use of compression for patients with lipedema [Stage 2,3]. All of the care guidelines recommend a multidisciplinary approach to treatment involving lymphedema therapists teaching patients manual lymphatic drainage, proper fitting compression garments, and instruction on the proper application of the lipedema garments. Therefore, we conclude that compression is usually needed in stage 1 lipedema and always needed in stage 2 and 3 lipedema.
What Is the Goal of Compression Pump Therapy in Lipedema?
The goal of compression therapy in lipedema is:
- Compression has been shown to reduce discomfort, aching and limb heaviness as well as supporting the health of the tissue.
- Compression helps to streamline uneven or distorted limb shape and improve movement.
- Compression helps to reduce edema by reducing the interstitial fluid formation and encourage venous and lymphatic return in lipedema. (Hardy, 2016)
All three goals are critical for the management of lipedema. Compression is the cornerstone on which all other treatments for lipedema are built upon as it is the only treatment that has been shown to benefit every patient with lipedema. Studies have shown medical grade graduated compression is the most universally applied effective treatment for reliving limb heaviness, tenderness and leg cramping and it should be the first line of treatment for lipedema as it is an extremely low risk and relatively low cost and readily available treatment. Compression with or without other lymphatic stimulating treatment are an effective first line of therapy for managing lobules, wrist and ankle cuffs that occur with lipedema.
St Louis Dr Wright Compression for Lipedema 4-8 23How Graduated Compression Likely Deters Progression of Lipedema
While the exact pathogenesis or pathogenic mechanism by which lipedema develops is not known, all current understanding points to the lymphatic system playing a role in the development and progression of lipedema and its symptoms. Medical grade graduated compression has not only been shown to treat symptoms of lipedema and correct lobules and ankle and wrist cuffs caused by lipedema, but also compression has been shown to optimize lymphatic flow and encourage draining of inflammatory interstitial fluid. The excess interstitial fluid and its inflammatory proteins and signaling agents seen with lipedema is responsible for nodular fibrosis, lobular fibrosis and progressive dermal fibrosis that occurs with lipedema. The progression of the fibrotic processes is highly linked to disability from lipedema.
The goal of compression pump therapy in lipedema is:
- To reduce discomfort, aching, and limb heaviness as well as to support the health of the tissue.
- Compression helps to streamline uneven or distorted limb shape and improve movement.
- Compression helps to reduce edema by reducing the interstitial fluid formation and encourages venous and lymphatic return in lipedema. (Hardy, 2016)
All three goals are critical for the management of lipedema. Compression is the cornerstone on which all other treatments for lipedema are built upon as it is the only treatment that has been shown to benefit every patient with lipedema. Studies have shown medical-grade graduated compression is the most universally applied effective treatment for relieving limb heaviness, tenderness, and leg cramping and it should be the first line of treatment for lipedema as it is an extremely low risk and relatively low cost and readily available treatment. Compression with or without other lymphatic stimulating treatment is an effective first line of therapy for managing lobules, wrist, and ankle cuffs that occur with lipedema.
Why is Compression Needed in All Stages?
Lipedema is characterized by painful and swollen fat which accumulates disproportionately in the subcutaneous tissue. New studies have shown that all stages of lipedema show increased swelling in the lower extremities as measured by Bioimpedance. In a study published this year in the Journal of Lymphatic Research and Biology, Crescenzi, Donahue, and Herbst showed that compared to controls all stages of lipedema have increased extracellular water or swelling. (R. Crescenzi, 2019) Further, the study showed that the edema or extracellular water increased with each stage of lipedema.
We know that extremity edema or lymphedema is associated with multiple inflammatory processes that are responsible for pain, tenderness and progressive fibrosis of the affected areas. All the Standard of Care [Dutch (Damstra, 2017), German, and British (Coppel, 2017)] Guidelines for the management of lipedema recommend the use of compression for patients with lipedema [Stage 2,3]. All of the care guidelines recommend a multidisciplinary approach to treatment involving lymphedema therapists teaching patients manual lymphatic drainage, proper fitting compression garments for lipedema, and instruction on the proper application of the compression garments. Therefore, we conclude that compression is usually needed in stage 1 lipedema and always needed in stage 2 and 3 lipedema.
How Graduated Compression Likely Deters Progression of Lipedema
While the exact pathogenesis or pathogenic mechanism by which lipedema develops is not known, all current understanding points to the lymphatic system playing a role in the development and progression of lipedema and its symptoms. Medical grade graduated compression has not only been shown to treat symptoms of lipedema and correct lobules and ankle and wrist cuffs caused by lipedema, but also compression has been shown to optimize lymphatic flow and encourage draining of inflammatory interstitial fluid.
The excess interstitial fluid and its inflammatory proteins and signaling agents seen with lipedema is responsible for nodular fibrosis, lobular fibrosis and progressive dermal fibrosis that occurs with lipedema. The progression of the fibrotic processes is highly linked to disability from lipedema.
Individual Recommendations for Compression with Lipedema
The optimal strength of compression depends on the individual patient and her stage of the disease. Of course, there are a few individuals with early Stage 1 lipedema who may not have any detectable interstitial edema or lymphedema who may not need medical-grade compression. Even this can be a bit tricky because most individuals with characteristic disproportionate fat consistent with early-stage lipedema are not symptomatic, so they may not technically meet the diagnostic criteria for lipedema.
These individuals still would likely benefit from compression garments. Perhaps; however, individuals with early symptomatic lipedema do not need medical-grade graduated compression and would suffice with compression garments that are not graduated or medical grade. Compression garments that are not graduated and were originally designed for post-operative recovery have a uniform compression strength of generally 12-20 mmHg.
The non-graduated post-surgical garments do not aid significantly in the flow of lymph. Compression garments sold by manufacturers like Solidea, Bioflect, Marena, and Veronique are very popular, but they are not recommended for any individual with symptomatic lipedema as they are not graduated and are not medical grade. Almost all individuals with lipedema have excess interstitial fluid or lymphedema and, therefore should be treated with medical-grade graduated compression applied to the areas of the body that are affected.
What Is Graduated Compression?
Graduated compression is based on the principle that fluid flows from higher to lower pressure. So to encourage the interstitial fluid or edema that builds up in lipedema to exit or flow out of the affected limbs the compression of the garments must be greater in the end, distal portion, of the limb and gradually lower pressure until the limb joins the body.
The principle of graduation is followed in the graduate garment such that maximal pressure or 100% compression strength is applied to the distal end such as an ankle or wrist, then 70% of the compression strength is applied to the calf or forearm. This gradually decreased pressure continues such that the knee or elbow has the approximate compression of the distal end and the thigh or upper arm usually has 30-40% of the maximum compression pressure. Almost all graduated compression is medical grade, which studies have shown the pressure strength measured in millimeters[mm] of Mercury [Hg] to be high enough to help moderate of higher edema.
What Pressure Are Considered Medical Grade and Recommended for Lipedema?
Medical grade compression strength varies by the affected limb and the severity of the edema or fluid accumulation. An arm requires less compression to aid lymph flow because it is both smaller than a thigh and closer to the heart so under less gravitational pressure difference. In general, 18 -20 mmHg [Mercury] is considered medical-grade compression for the arm and 30 – 40 mmHg strength at the ankle is considered a medical-grade compression strength for the leg. These recommendations are based on studies primarily of primary lymphedema as this is the strength required to cause a significant improvement in lymphatic flow. (Mosti, 2019) The studies of compression garments show those [e.g. 30-40 mmHg ankle and 18-20 mmHg wrist] pressures give both optimal venous blood flow and lymphatic fluid clearance from the affected limbs.
Sometimes compromises are made, and lower 20-30 mmHg compression is used for individuals who have very mild edema or who are just starting to use compression garments or because of extreme sensitivity to the pressure of the compression. Ideally, the lower 20 -30 graduated compressions are used as a stepping-stone until the heavier compression can be tolerated because the evidence for this lower strength of graduated compression controlling interstitial fluid is much weaker and not as trustworthy.
While it is yet to be proven that proper compression can reduce the progression of the lipedema at this time, the recommended graduated 30-40mmHg pressures at the ankle have been shown to be effective at minimizing edema, reducing symptoms and halting the progression of the disease in closely related lipedema, veno-lymphedema, and other diseases that are known to cause secondary lymphedema and therefore 30-40 mmHg strength at the ankle must be the goal of compression therapy.
Compression Physiology and How Compression Works in Lipedema
When considering the use of compression therapy in the management of lipedema, the basic principles should be understood. The law of Laplace is a mathematical formula that defines the 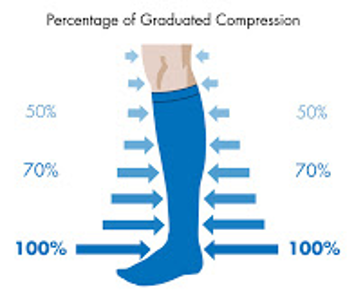

The law of Laplace
P relative to N T/R
P = pressure
N = number of layers T = tension applied = radius of limb
Special Needs and Flexibility with Compression in Lipedema
Compression garments are hard to fit for women with Lipedema. By definition, the fat accumulates out of normal proportion on the bodies of individuals with lipedema, which leads to unique body shapes. Often hips, thighs, and calves will be much larger on individuals compared to the rest of their bodies. These size differences necessitate flexibility with compression garments and layering of multiple compression garments.
One of the most successful combinations for coverage of the legs is to get knee-high socks with 30-40 mm Hg compression strength at the ankles and layer it with Capri length compression pants that overlap at the top of the calf. This combination gives a comprehensive coverage for the entire lower extremity without gaps. Another combination that is very effective for patients with lipedema is thigh-high compression stocking layered under compression shorts that go to the top of the knees. The compression shorts help hold the thigh stockings in place. Not only does the layering of the garments help hold the garments in place it also allows for the garments to be different sizes.
Compression Garments
Lipedema is a condition that, should it be allowed to progress, can become a very serious medical problem. Lipedema and lymphedema cannot be cured, so the focus for treatment is on procedures that can minimize the swelling, control the associated pain, and prevent the disease from getting out of control.
One of the main treatments in the arsenal of tools that can be used to treat these conditions is compression. In addition to other treatments, compression can be very effective in containing the symptoms of lipedema. Compression garments are generally prescribed to lipedema sufferers following decongestive therapy to help maintain the reduction of swelling. Compression therapy will also help encourage the flow of the lymphatic fluids out of the affected limb.
Compression garments are to be worn 24 hours a day, every day. Because of this, it is important that patients are fitted correctly and use the best type of compression garment for their individual cases. An inaccurate fit or a poor quality garment can cause additional pain and discomfort.
Why Compression Garments?
There are many reasons to consider using compression garments. The underlying problem with all lymph disorder is problems circulating lymph back to the venous system. For individuals who have lipedema, are doing compression treatment for lymphedema or lipo-lymphedema, compression garments are often used to assist the lymph circulation by increasing the pressure in the tissue propel lymph fluid through the body. Lymphedema causes excess fluid to become trapped in the extremities, especially the legs, and compression garments put pressure on the skin and veins, helping them clear lymph and decongest.
Besides improvement to lymphatic flow, there is some debate about compression garments’ and compression therapy benefits related to fat disorders, such as Lipedema. Most people with lipedema the pain tenderness are worsened by swelling and activities such standing or having the legs hand dependent that promote local swelling. Compression garments can help reduce pain and heaviness felt in the limbs from fat disorders such as lipedema by decreasing swelling in the fat and throughout the limb. Also compression potentially reduces the rate at which the fat cells grow and help to prevent fat disorders from progressing to more serious stages. In other words, compression can be one of the best treatments for lipo-lymphedema or fat caused by lymphatic diseases.
Types of Compression Garments
There are many different types of compression garments to choose from, all designed to provide slightly different benefits. You will want to discuss which type of compression garment is appropriate for you with your doctor.
Circular & Flat Knit
These compression stockings, typically made of nylon or nylon-cotton blend, are thin stockings with multiple angles of stretchiness. Circular knit garments stretch along both the length and width of the garment, while flat knits have a seam and only stretch two directions. Large and abnormally shaped limbs typically see more benefits from flat knit style garments; additionally, flat knit’s thicker design provides a slightly more comfortable fit.
Inelastic
These garments, made from non-stretch material, mimic the effects of bandage wrapping techniques. The thought process behind use of inelastic garments is that preventing swelling requires a garment that cannot be stretched. While other types of compression garment allow the limb a small amount of stretching, inelastic garments use Velcro to lock into place.
Micro Massaging
The micro massaging compression garments use a textured knit material to micro massage the lymphatics through movement of the top layer of skin. As you move in these garments, it stretches the top layer of skin, massaging the lymphatics below. These garments have the lowest compression and the most stretchiness of any compression garments, and it is debated whether the micro massaging benefit outweighs the lack of a stronger compression. In early lipedema the micro massaging compression garment like bioflex can provide good relief.
Nighttime
For some patients, wearing compression garments throughout the day is not wholly effective. For these patients, nighttime garments can help. These are thicker padded garments aimed at reducing nightly swelling and breaking up fibrotic tissues. Frequently made with spandex wicking fibers, these garments take some time to get used to, as their bulkiness can be disruptive to sleeping for new wearers.
Pneumatic Compression Pumps
For many people who suffer from lipedema or lymphedema, the symptoms can be uncomfortable and difficult to manage. Lymphedema causes fluid buildup, especially in the limbs, due to the lymphatic system’s inability to properly drain the fluid back into the core. Certain therapy methods, including the use of compression garments and Complete Decongestive Therapy, have been shown to be effective at treating lymphedema (and in many cases, lipedema). One option patients have to manage their own symptoms at home is pneumatic compression pumps.
How Compression Garments Work
Pneumatic compression pumps are a great at-home solution for patients suffering from lipedema (British Spelling: Lipoedema) or lymphedema. Following the same principles as Complete Decongestive Therapy, pneumatic compression pumps are devices that mimic the massage techniques used in manual lymphatic drainage. An intermittent pneumatic compression device (IPC) is worn on the affected limb and activated to help push retained fluids back towards the core of the body. These devices let patients who may have difficulty or are unable to visit a doctor’s office often still find relief from their symptoms.
Benefits of Pneumatic Compression Pumps
There are many compression therapy benefits to having your own pneumatic compression pump. If you have compression stockings to help mitigate symptoms from lymphedema, but they aren’t providing enough relief, an intermittent pneumatic compression device can help you get daily treatment. Combating with compression therapy for lymphedema involves a constant focused effort to see results, and an IPC helps you to keep up with treatments at home, without having to visit the doctor’s office often.
Complete Decongestive Therapy often utilizes IPC devices to assist in the treatment of patients. CDT treatments are very effective at treating extreme levels of lymphedema, and IPC devices help patients to continue their treatment at home and keep their lymph fluid from rebuilding in the affected limbs.
Consider an IPC Device Today
If you’re having issues controlling your lymphedema symptoms, talk to your doctor about pneumatic compression pumps today. These useful devices can help you alleviate symptoms at home using the same principles as decongestive therapy massage used by top physicians. Schedule a consultation today to see how an IPC device could help you overcome the issues caused by lymphedema.
For more information on Lipedema please visit FatDisorders.org for some valuable information.
→Up Next: Dry Brushing & Vibration
What Diet is the Best for Lipedema?
The best diet for lipedema is The Rare Adipose Disorder (RAD) Diet, a modification of the Mediterranean diet. You can learn more about it here.
References:
Best Practice Guidelines: The Management of Lipoedema. Wounds, UK, 13(1), Vol 13, No 1. Retrieved from https://www.lipoedema.co.uk/wp-content/uploads/2017/05/WUK_Lipoedema-BPS_Web.pdf
https://www.ncbi.nlm.nih.gov › books › NBK545818
Damstra, R. (2017). The Dutch Lymphedema Guidelines Based on the International Classification of Functioning, Disability, and Health and the Chronic Care Model. Journal of Vascular Surgery: Venous and Lymphatic Disorders, 5(5), Vol. 5, Number 5. doi:www.ncbi.nlm.nih.gov/pubmed/28818234.
https://www.ncbi.nlm.nih.gov › pubmed
Hardy, D. (2016). Best Practice Guidelines for the Management of Lipoedema. British Journal of Chronic Edema, https://www.ncbi.nlm.nih.gov/pubmed/28961048. Lipoedema: presentation and management
Mosti, G. (2019). Compression Therapy in Lymphedema: Between past and recent scientific data. Phlebology, 34(8), 518-522. Compression therapy in lymphedema: Between past and recent scientific data
- Crescenzi, P. D. (2019). Lipedema and Dercum’s Disease: A New Application of Bioimpedance. Lymphatic Research and Biology, 10.1089/lrb.2019.001. Research Impact








