Choose Your Liposuction Surgeon Carefully
After you’ve been officially diagnosed and are ready to put a treatment plan together, you must partner with a surgeon you trust. By the time most women are aware of their disease, their lymphatic circulation has already become significantly impaired. Because liposuction can further injure the lymphatics, extra care must be taken to avoid injury to lymphatic flow and function during your procedure. Detailed knowledge of lymphatic anatomy and a careful surgical technique designed to minimize the risk of injury to the lymphatic structures is required.
Liposuction surgeries are often referred to as lymph sparing liposuction and require very different skills than those used in general liposuction. So, how can you be sure that the surgeon you are considering has the expertise to give you optimal improvement with your lipedema and the lowest chance of complication? We recommend asking the following questions:
- How long has your prospective surgeon been performing liposuction for patients with lipedema?
- What criteria does the surgeon use to diagnose lipedema?
- Does he or she offer to diagnose lipedema via Skype without a physical exam?
- Does the surgeon follow the standard lipedema guidelines for a multidisciplinary approach to the treatment of lipedema?
- What surgical techniques does your prospective surgeon use to avoid injury to the lymphatics?
- Does the surgeon you are considering participate in research or registries to track outcomes and prove the benefits of the liposuction surgery they perform?
If your surgeon does not have answers readily available to these questions, we highly recommend you continue researching other options.
Reliable Lipedema Surgical Outcomes
How does the surgeon determine the outcomes of his or her surgery, and how do they follow-up with their patients? If the surgeon does not follow-up with their patients post-liposuction, they cannot know for sure if there were complications. Far too often surgeons do not follow-up on patient improvements or complications. So, if they claim to have no complications in their surgical history, you’ll want to make sure they have a strong and consistent follow-up process. If they don’t follow-up, they are tracking their post-procedure complications.
Spanish Standard of Care- Lipedema Guidelines:
According to the Spanish Standard of Care Guidelines:
The surgical treatment of lipedema has become, in the last decade, the only definitive treatment option for these patients, present in clinical lipedema guidelines and protocols. Its main objective is the reduction of the fatty compartment by reducing the circumference and volume of the extremities.
Prior to surgical treatment, associated aggravating factors such as edema, obesity, unhealthy lifestyle, or lack of physical activity should be corrected.
In liposuction, small incisions are made in the skin for the introduction of the cannula. These incisions are 2-4 mm and are performed in the most appropriate locations for the removal of fat.
“The liposuction technique in lipedema is different from conventional techniques. Thinner and blunt cannulas are used, and liposuction must follow an axial or longitudinal pattern, and not transverse as usual in traditional liposuction. The objective is to minimize the potential lesions of the superficial lymphatic system” (Mladick R, 1990).
“The perfect anatomical knowledge and the correct execution of the technique are essential to reduce the possibility of complications, in specific areas such as ankles and knees.” (Frick A, 1999).
It is a sequential treatment, because to achieve satisfactory results and maintain safety criteria, it is necessary to perform an average of 2 or 3 interventions, with a variable range between 1 and 6.
Dutch Standard of Care Guidelines:
According to the Dutch Standard of Care Guidelines published on Phlebology: The Journal of Venous Disease and the US National Library of Medicine:
This technique has been proven to be a highly effective treatment for lipedema with positive morphological and functional long-term results, including the reduction of complaints, such as pain and bruising, and enhanced overall quality of life. [1], [2], [3], [4] Consistent criteria to determine the ideal time or patient characteristics for liposuction are not available. Some studies report better outcomes in the early stages compared with advanced cases, but recent data demonstrate a more distinct change of complaints in more advanced cases.
Ideally, TLA is performed at a relatively early stage to prevent progression. [2], [4] The lipedema guidelines task force recommends tumescent liposuction as part of the therapeutic armamentarium in the management of lipedema. However, tumescent liposuction is only the treatment of choice for patients with a suitable health profile and/or inadequate response to conservative and supportive measures.
German Standard of Care Guidelines:
According to the German Standard of Care Guidelines published on the Wiley Online Library and on the Association of the Scientific Medical Societies in Germany:
Liposuction is used for the permanent reduction of abnormal subcutaneous fat on the arms and legs. It is especially indicated when despite consistently carried out conservative therapy, symptoms still remain or there is a progression of findings (subcutaneous fat volume) and/or symptoms (pain, edema) (Cornely 2000, Schmeller 2014).
Due to its many advantages, liposuction should be carried out using tumescence local anaesthesia (TLA), i.e. a “wet technique” with blunt micro-probes (Klein 2000, Sattler 1997 & 2002, Rapprich 2002 & 2011, Cornely 2003 & 2006, Schmeller 2007). Supporting techniques such as vibration or water jets can also be used (Stutz 2009). This procedure can be carried out as an outpatient or inpatient (Schmeller 2012, Rapprich 2011, Cornely 2014).
Furthermore, due to the reduction of fatty tissue deposits on the inner sides of the upper leg and knee, mechanical and occlusive related skin damage is reduced or eliminated. Correction of leg deformity leads to improvement of movement and gait (Stutz 2011), as well as risk reduction for further orthopedic complications as a consequence of lipedema-associated pathological gait.
British/ UK Standard of Care Guidelines:
According to the UK Standard of Care Guidelines published on Lipoedema UK:
Liposuction should be carried out by a surgeon who is appropriately qualified to treat someone with lipoedema and who works as part of a multidisciplinary team.
Patients should research clinics carefully to ensure an adequate standard of care and to establish that the procedures on offer are appropriate for their individual needs. They need to be aware that liposuction procedures are not without risk in the immediate postoperative period and may cause long-term complications (Stutz & Krahl, 2009; Rapprich et al, 2015).
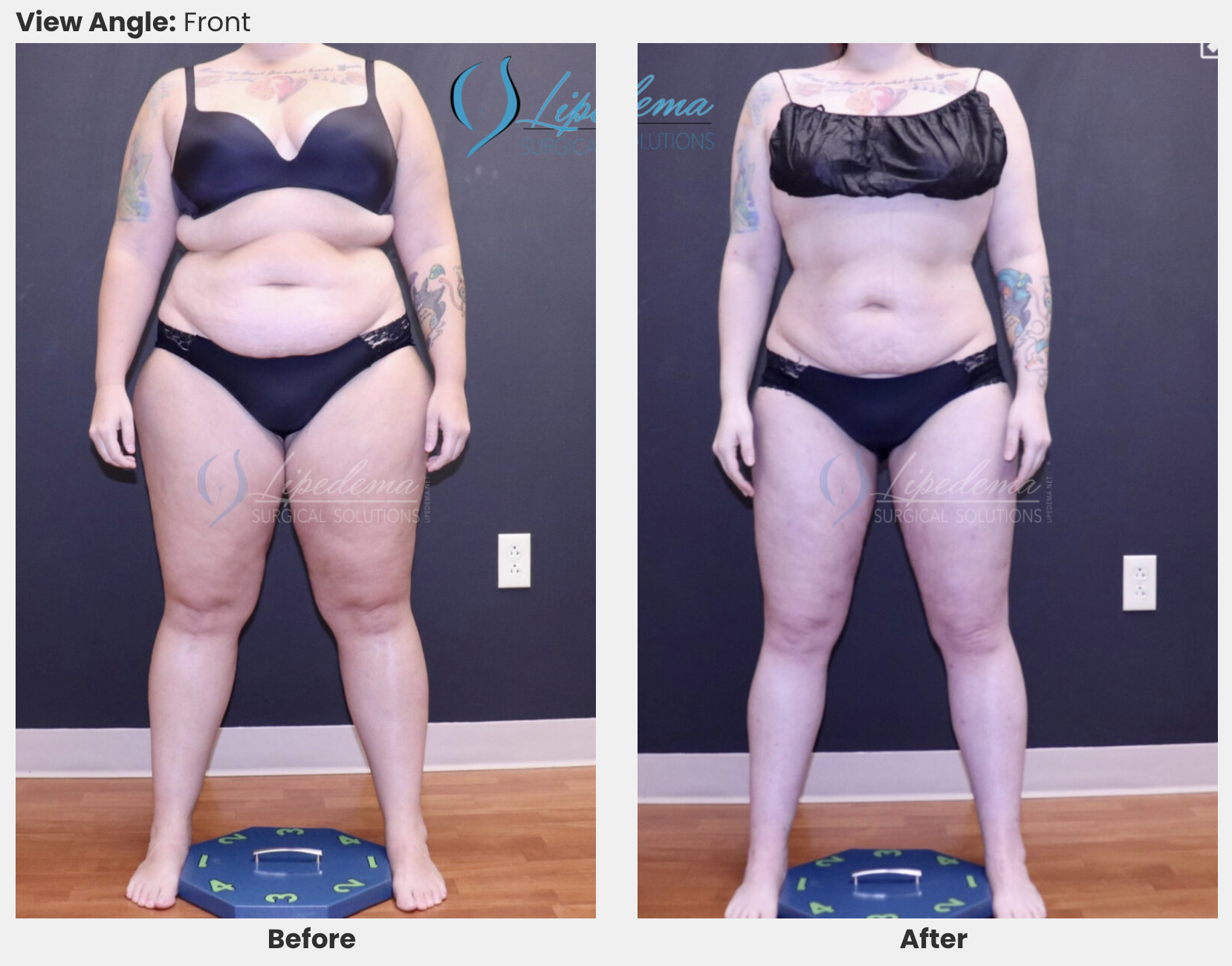
Effects of Liposuction in Lipoedema
Overall, liposuction in patients with lipoedema reduces tissue bulk, pain and bruising, and improves mobility, functioning and quality of life (ReichSchupke et al, 2012; Peled & Kappos, 2016). A study of tumescent liposuction in 85 patients with lipoedema found that six months after surgery patients’ scores for a wide range of symptoms, including pain, bruising, swelling and impaired mobility, were all significantly reduced in comparison with preoperative scores (p<0.001 for change in each item score) (Rapprich et al, 2015). Patients received a mean of 2.61 (range 1 to 6) sessions of liposuction.
There is also evidence of longer-term benefits of liposuction. A study sent a questionnaire to 112 patients who had undergone tumescent liposuction between 5 and 11 years previously and who had also been evaluated by questionnaire four years before (Schmeller et al, 2012; Baumgartner et al, 2016). Responses were received from 76% of patients. Changes over time in seven parameters (including pain, bruising, oedema, mobility and quality of life) that contributed to an overall impairment score were examined. The significant reductions in pre-operative and post-operative scores for each item and for overall score (all p<0.001) noted at 4 years were also present after 8 years (Schmeller et al, 2012; Baumgartner et al, 2016). However, studies are awaited that present data for the longer-term outcomes that are relevant for this patient group.
Advising Patients with Lipoedema
Patients with lipoedema considering liposuction should be advised and encouraged to undertake non-surgical treatment for at least 6-12 months as a first step. Pre-operative counseling is very important to ensure that the patient has realistic expectations of what can be achieved, understands the procedure and the importance of post-operative care (including compression therapy), and comprehends that there is no evidence that liposuction is curative.
Summary and Conclusions – Lipedema Guidelines
The disease lipedema presents some unique issues with regard to its management. In the USA, the recognition, understanding, and treatment of lipedema are inconsistent by the majority of physicians and surgeons. Patients with lipedema need to do their research to find surgeons who perform lymph sparing liposuction and who are dedicated to following the standards of care, lipedema guidelines, and comprehensively treat lipedema patients. In the proper multidisciplinary teams hands, liposuction and lipedema weight loss success can significantly improve the symptoms, quality of life and mobility of patients with lipedema.
References:
- Forner Cordero I, Szolnoky G, Forner Cordero A, et al. Lipedema: an overview of its clinical manifestations, diagnosis and treatment of the disproportional fatty deposition syndrome – systematic review. Clin Obes 2012; 2: 86–95 https://www.ncbi.nlm.nih.gov/pubmed/25586162 or Google Scholar Link
- Langendoen SI, Habbema L, Nijsten TEC, et al. Lipoedema: from clinical presentation to therapy. A review of the literature. Br J Dermatol 2009; 161: 980–986. https://www.ncbi.nlm.nih.gov/pubmed/19785610 or Google Scholar Link
- SchmellerW, Hueppe M and Meier-Vollrath I. Tumescent liposuction in lipoedema yields good long term results. Br J Dermatol 2012; 166: 161–168. https://onlinelibrary.wiley.com/doi/abs/10.1111/j.1365-2133.2011.10566.x and https://www.ncbi.nlm.nih.gov/pubmed/21824127 or Google Scholar Link
- RapprichS, Dingler A and Podda M. Liposuction is an effective treatment for lipedema – results of a study with 25 patients. JDDG 2011; 9: 33–40. https://www.ncbi.nlm.nih.gov/pubmed/21166777 and https://onlinelibrary.wiley.com/doi/abs/10.1111/j.1610-0387.2010.07504.x or Google Scholar Link
- Peled AW, Slavin SA and Brorson H. Long-term outcome after surgical treatment of lipedema. Ann Plast Surg 2012; 68: 303–307. or Google Scholar Link: Long-term Outcome After Surgical Treatment of Lipedema
and https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4986968>/ or Google Scholar Link - Meier-Vollrath, Iand Schmeller W. Lipoedema – current status, new perspectives. JDDG 2004; 2: 181–186. https://onlinelibrary.wiley.com/doi/abs/10.1046/j.1439-0353.2004.04051.x and https://www.lymfoedeem.nl/ or Google Scholar Link
- Buck DW, Herbst KL. Lipedema: a relatively common disease with extremely common misconceptions. Plast Reconstr Surg Glob Open. 2016;4(9): e1043. https://www.ncbi.nlm.nih.gov/pubmed/27757353. and https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5055019/ or Google Scholar Link