Hello to everybody! My name is Cat, and I’m a patient of Dr. Wrights, and a writer and content creation in the Women’s Health space. Dr. Wright and I work closely together, and I’ve put together some helpful information to give you the high points of the Lipedema treatment journey.
Everything You Need To Know About Lipedema, from 1 Lippy Lady to Another
For the first 29 years of my life, I walked through the world with the bitter understanding that I would never have a body I could be proud of. I became resolved to the fact that even though I live in Austin, Texas, where we average 300 days of sunshine and 8 months of 90-100 degree heat, shorts would never be a comfortable option for me. And in the few months of cold, boots over my shins were out of the question. What a cruel joke, right? In the summers I’m too hot, and in the winters I’m too cold.
After decades of rigorous diet and exercise, strict calorie counting, and perfect attendance at my accountability groups, I was at a complete loss. How could my body take me across the finish line of a half marathon, yet it couldn’t shed a single pound through my training? And how are my legs and butt this outrageous? Sure, there are perks to a body shape that most people envy, but only at the cost of extreme self-consciousness, depression, and intense leg pain and bruising. And how can every diet I try have absolutely zero permanent effects on my weight? Is that even scientifically possible? As it turns out – it is. Below is me in Dr. Wright’s office for my original diagnosis. I flew in for a morning appointment and flew home that night. What a whirlwind!


If you’ve made it to this website, I’m so happy you’re here! This means you’ve magically stumbled upon the answers that our doctors never told us – maybe they didn’t know, maybe they didn’t care to know, or maybe they were blinded by their very typical diagnosis of obesity (or lymphedema, or venous insufficiency, or some other incorrect thing). But as we dig into Lipedema and everything you need to know about it, I welcome you with a virtual hug, and I encourage you to take a moment to celebrate.
You are not crazy.
You are not simply ‘obese’.
It’s not your fault.
You are not alone.
And if knowledge is power, my dear friend, you are about to be the most powerful you’ve ever been!
What is Lipedema?
Evil.
And a subcutaneous fat disease that primarily affects women. When we reference the ‘subcutaneous” tissue and fat, we’re referencing the layer of tissue directly under the skin.
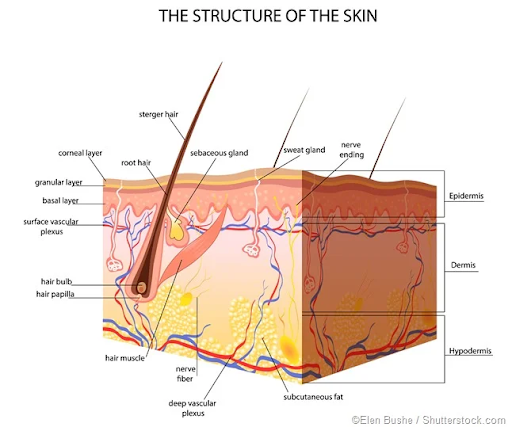

Shockingly, Lipedema affects an estimated 17 million women across the globe. When I said you weren’t alone, I wasn’t kidding! This disease affects a huge number of women, the majority of whom are still walking through their world the way I was walking through mine: lost, sad, and in a lot of physical and mental pain. Lipedema is a disease that leads to the excessive build-up of fat cells, primarily in the arms and legs. Women suffering from it often have “pockets” of fat on their limbs that appear disproportionate in comparison to the rest of their body. This disease causes an enlargement of the legs due to deposits of fat under the skin, and typically gets worse over time, making diagnosis and treatment essential.
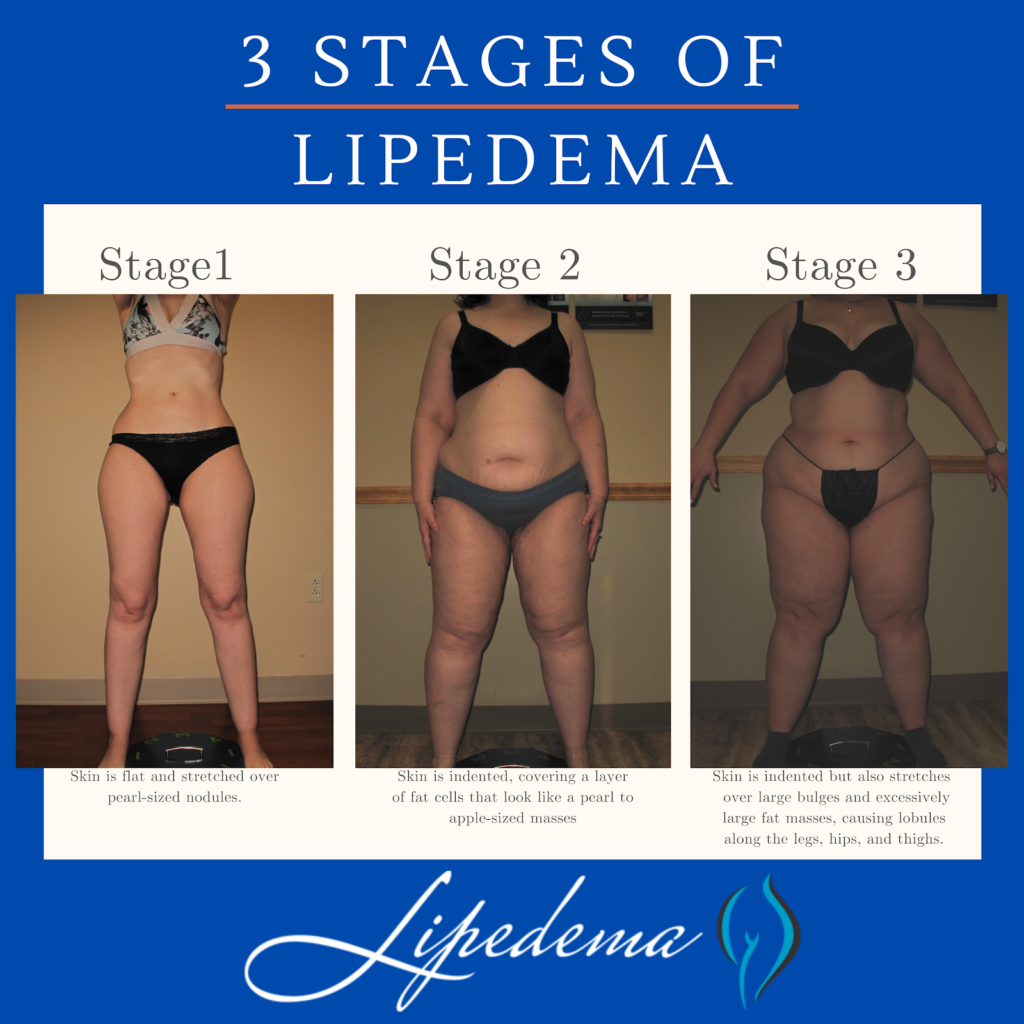

I personally had an extremely tiny waist, wore a size small top, and XL or XXL bottoms. My arms were mostly unaffected until my late 20s, but my legs were large, heavy, and totally disproportionate from the time I was 12 years old. What 12-year-old has already developed a pear-shaped body? Lipedema 12-year-olds, unfortunately. Pockets of fat developed in my legs and appeared to bulge in and out. The fatty bulges that I used to think were just extremely bad cellulite were actually pockets of Lipedema fat all over my thighs.
These pockets of Lipedema fat are accompanied by painful symptoms, such as excessive swelling, pain, numbness, and very easy bruising. If my dog jumped up on my legs, it was excruciating. If I bumped my hip into the side of a table, I knew I’d wake up with a deep, painful bruise the next day. As Lipedema progresses over time, these symptoms will continue to get worse as more Lipedema fat accumulates, and many women report that they are less and less mobile or active as time goes on. As a result, these women are stuck in a terrible cycle; they are less mobile, so they often gain weight, then it’s even more difficult and painful to be active, and the cycle goes on and on.
With Lipedema, we experience fat accumulation in specific areas, which may help indicate if your weight gain is normal or not. If you’re gaining pockets of fat that are out of proportion to other areas, this may be a tip-off that you have Lipedema.
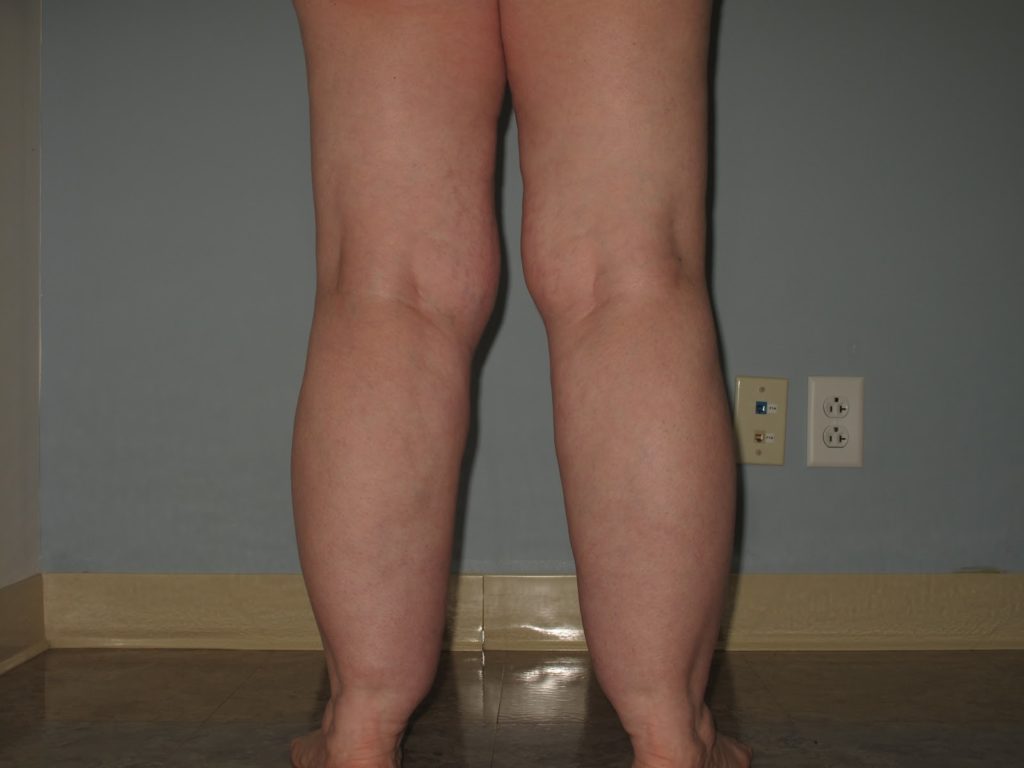

While many women also see weight gain in their arms, it’s common that the following areas are greatly affected:
- Cankles: an accumulation of fat around the back of your ankles, causing an “ankle cuff.” This type of weight gain is a clinical sign only seen in Lipedema. Not all patients get this, but if you have it, it may be an indicator.
- Bat Wings: Weight gain in your upper arms, causing a “bat win” effect. This is seen in about 80% of women with Lipedema.
- Saddle Bags: Large areas of fat that project outwardly beyond the normal curve of your hip, also known as “football saddlebags” (because they look like there’s a football on the sides of your hips).
Buttock Self: This is a larger buttock that sticks out significantly from the lower back when looking at your silhouette from the side. This is another feature seen in most women with Lipedema.
What Causes Lipedema?
This is where things start to get really exciting. It was only in mid-2019 that my research brought me to Lipedema, and at the time of my first surgery to treat it (in December 2019), there was still very little known about the causes. Experts in the field had hypothesized that the disease was hormonal in nature and very likely had a genetic component, but research was still too early to tell. But for all the doom and gloom 2020 has brought the world, we’ve also seen some really big and exciting movement in understanding the cause of this enigmatic disease.
We know that Lipedema is inherited in about 60% of women, likely through genetics, and is the result of a malfunction of the Lymphatic System. The lymphatic system is a network of tissues and organs that help rid the body of toxins, waste, and other unwanted materials. This system transports lymph fluid throughout the body and is important for maintaining a healthy immune system. This disease affects the lymphatic system’s tiny vessels (microvessels) that cause a build-up of excess fluid around the body’s tissue cells. These tissue cells (located in the subcutaneous layers we discussed above) are then full of excess fluid, causing the swelling, soreness, bruising, and pain that many women with Lipedema report.
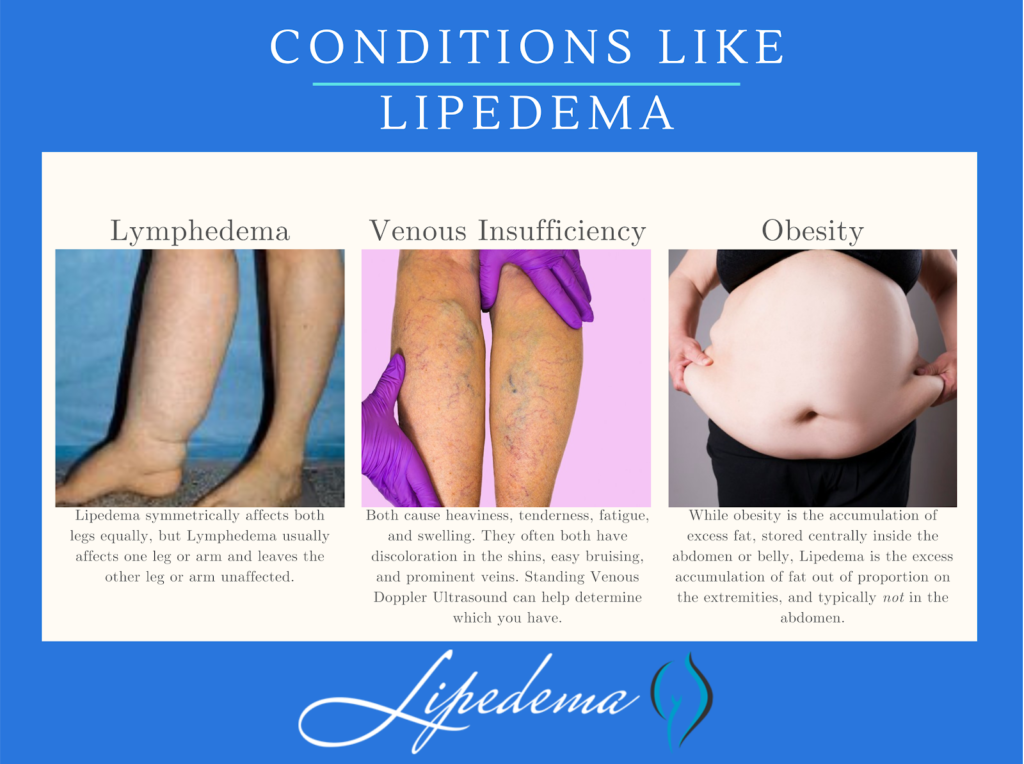

Researchers now also have evidence that suggests there are specific biomarkers of this specific lymphatic malfunction that will provide medical providers a way to recognize – in our DNA – the differences between lymphedema, lipedema, obesity, and other potential lymphatic diseases.
But why is that so exciting? Just because we know what causes it doesn’t make it hurt less, right? Well, that’s kind of true, but kind of not! As researchers continue to gain understanding and genetic proof of Lipedema and differentiate it genetically from other diseases that we’re commonly misdiagnosed with, it will only become easier for women with Lipedema to get a proper diagnosis. Then, as the disease is more widely known and understood, treatments will become better and better, it will be more difficult for insurance providers to refuse coverage for treatments. Hopefully from there, more doctors will be trained in treating women with Lipedema properly, so treatments will become more accessible across the country!
While it’s true that the disease itself is still painful and terrible, getting the research out there will allow for a much earlier diagnosis than women with Lipedema are used to. While I’m frustrated that it took me 30 years to get a diagnosis, I’m actually one of the lucky ones. Most women aren’t diagnosed until much later in life, well into their 50s, 60s, and even 70s. This advancement could be the beginning of the end for that trend!
How do you treat Lipedema?
There are two categories of treatment, surgical and non-surgical. During my first visit to Dr. Wright’s office after being officially diagnosed, we first put a non-surgical treatment plan together so that I could start it right away. After that, we went through my surgical treatment plan because I was already in an advanced stage. Today, I’ve completed 2 of my 5 scheduled surgeries, with a delay thanks to the COVID-19 pandemic. I’m so grateful that we went through both treatment plans because I am now back to practicing my non-surgical treatments while I wait for my next surgery. Both are necessary, especially because Lipedema is a progressive disease! Even after my surgeries are complete, I’ll be continuing with the non-surgical practices for the rest of my life. Below is one of the first full body photos I’ve ever taken of myself, shortly after healing from my 2nd surgery.


Non-Surgical Treatment Options
To the dismay of patients, wearing medical-grade, tight compression garments 24-hours per day, seven days per week, is the key to improve circulation for the lymphatic system, making this a go-to prescription from Lipedema experts. Compression garments come in a variety of strengths and will be prescribed based on the stage and type of affected areas. The tighter the compression, the better.
A healthy and consistent lifestyle of clean eating and low-impact exercise to address obesity will also help with Lipedema. A diet focused on low-carb and low-sugar has proven successful. Low-impact exercise such as walking, water aerobics, yoga, or gymnastics has also reported success. Patients must avoid yo-yo dieting while also permanently losing or, at the very least, maintaining their weight. What works for one patient may not work for another. Diet and exercise recommendations and healthy practices are essential, but ultimately should be based on the individual with the understanding that weight gain is not an option.
Some patients opt-in to Manual Lymph Drainage massage (MLD), a gentle skin massage used to stimulate the circulation of the lymphatic system. While experts have yet to find significant evidence that MLD helps with Lipedema directly, some patients prefer it for its “hands-on” nature to addressing their symptoms.
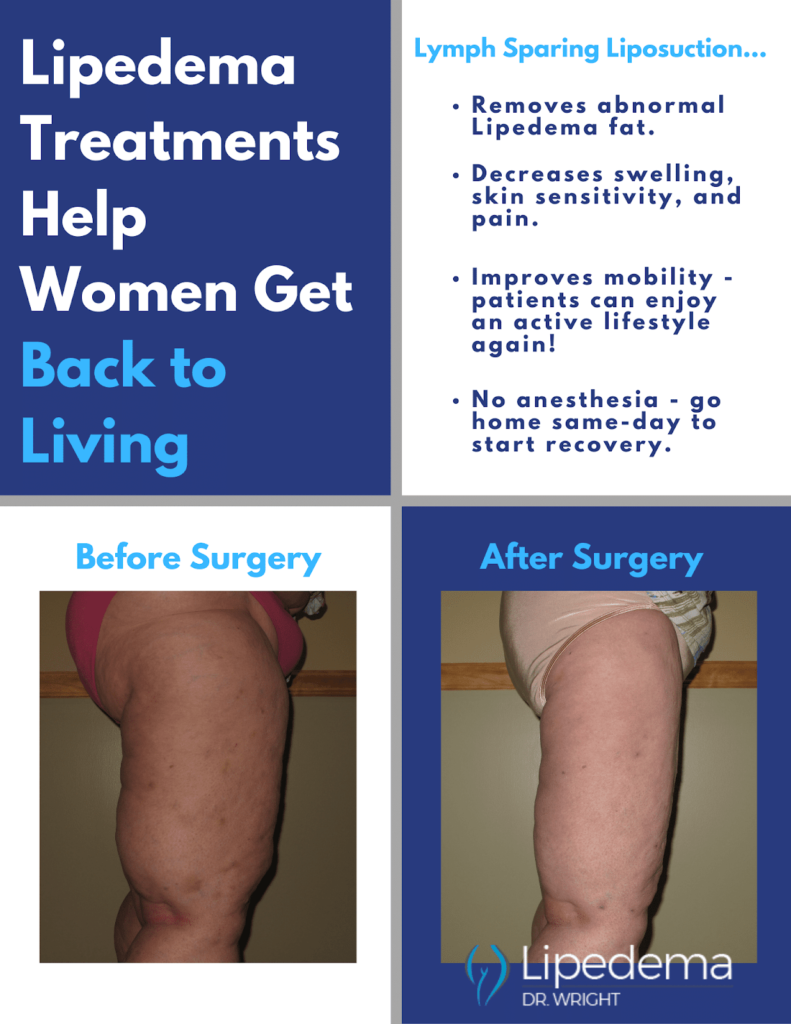
Lymph-Sparing Liposuction for Lipedema
For patients in the later stages of Lipedema, the pain and disruption to daily life are not permanently addressed with compression garments, diet, and exercise alone. Traditional liposuction that uses general anesthesia, radio frequencies, ultrasound, or lasers are possibly damaging to the lymphatic vessels, and as such are not an option for Lipedema patients, either. However, Lymph-sparing liposuction is safe, using surgical techniques that avoid lymphatic injury, and the use of local tumescent anesthesia reduces the risk of complications. Generally, the most painful areas should be treated first, starting high on the legs and then moving downward in future surgeries.

How Do I Start Getting Treatment for Lipedema?
I can confidently say that you’ve already done the most difficult part of this Lipedema journey – you lived with it without any answers! Now, it’s time to work on getting a formal diagnosis and working with your medical provider on what plans and timeline will work best for you. Review our 4-Step Guide to Getting a Lipedema Diagnosis, and as always, reach out to Dr. Wright if you have any questions! His website is a wealth of resources and knowledge, and he’s truly passionate about furthering the treatment and research to help women like us (I speak from experience!).






