

As we ring in the new year, the world continues to create find new normals in a pandemic as the coronavirus variants keep us on our toes. As we now well know, people of any age and gender can be infected with COVID-19, but there are a number of conditions that make individuals more likely to get severely ill from the virus. New research has shown that the risk of severe COVID-19 increases as the number of underlying medical conditions increases in a person and that individuals with an increased amount of fat in their bodies are at an increased risk of contracting the coronavirus, and may also suffer from a severe illness and side effects than those with lower body fat.
Severe illness means that a person with COVID-19 may:
- Be hospitalized
- Need intensive care
- Require a ventilator to help them breathe
- Die
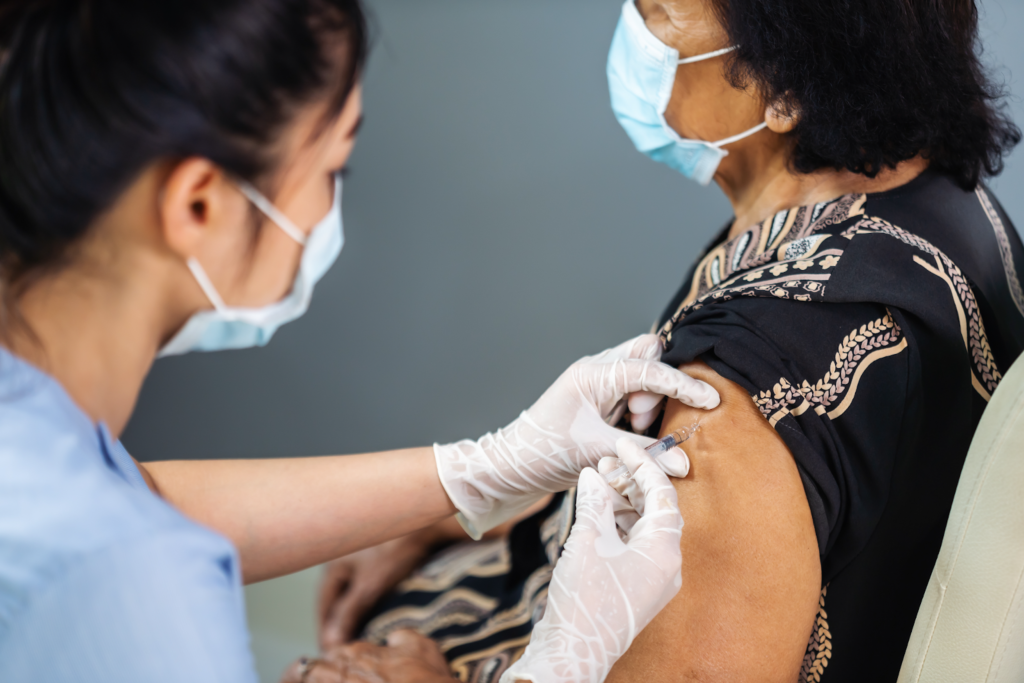
As a result, women with lipedema – who are prone to hold higher levels of fat on their bodies – are highly encouraged to take all precautions against COVID-19, especially by getting both vaccinated and boosted.
What is Lipedema?
Lipedema is a rather common, yet often painful disorder that affects the accumulation of fat cells in the body. While fat cells, otherwise referred to as adipose tissue, are an important feature in providing the human body with both cushioning and insulation. Lipedema causes the excessive congregation of these cells, particularly around the legs. Sometimes, spreading occurs in the torso, and in many cases, excessive clustering of fat cells is noticed in the arms as well. It’s estimated that arms are affected in nearly 80% of Lipedema cases reported.


Who is Affected by Lipedema?
Women tend to be the vast majority of individuals affected by Lipedema. It is estimated that at least 11% of women worldwide suffer from this disorder. Because Lipedema is highly resistant to both diet and exercise regimens, it’s not uncommon for women suffering from Lipedema to be misdiagnosed with either traditional obesity or lymphedema.
Symptoms and Stages of Lipedema
Lipedema can be noticeably characterized by the excessive and disproportionate appearance of nodular fat accumulations across the legs, hips, thighs, and often arms. Unlike Lymphedema, Lipedema has a tendency to affect both limbs equally and generally becomes more apparent over the course of time. It’s common for those who suffer from Lipedema to bruise rather easily as well.
Overall, Lipedema appears in a series of three stages. Stage 1 presents in patients as skin that is flat stretched over pearl-sized nodules that show up within a layer of fat showing increased cell size. Stage 2 presents as indented skin that’s covering a layer of fat cells presenting as a pearl to apple-sized masses. Stage 3 presents as pearl-sized nodules in combination with excessively large fat masses causing lobules along the legs, hips, and thighs and frequently extending to the torso or upper arms.
Lipedema & COVID-19
The Center for Disease Control has determined that as an individual’s BMI increases, so do their chances of a more severe case of COVID-19 if contracted. Overweight (defined as a body mass index (BMI) ≥ 25 kg/m2 but < 30 kg/m2), obesity (BMI ≥ 30 kg/m2 but < 40 kg/m2), or severe obesity (BMI of ≥ 40 kg/m2), can make you more likely to get severely ill from COVID-19.

Body Mass Index (BMI) is a calculation that illustrations the relationship between a person’s weight and height, and equips healthcare providers with one tool in evaluating a patient’s overall health. Specifically, these ranges are used to categorize whether a person is underweight, in a normal weight range, overweight, or obese. While BMI does not provide the full picture of a patient’s health or the full body composition breakdown, it is a commonly used factor in diagnosing numerous diseases.
The risk of severe COVID-19 illness increases sharply with elevated BMI.
A study of COVID-19 cases suggests that risks of hospitalization, intensive care unit admission, invasive mechanical ventilation, and death are higher with increasing BMI. The increased risk for hospitalization or death was particularly pronounced in those under age 65. More than 900,000 adult COVID-19 hospitalizations occurred in the United States between the beginning of the pandemic and November 18, 2020. Models estimate that 271,800 (30.2%) of these hospitalizations were attributed to obesity.
Lipedema vs. Obesity
While Lipedema is metabolically the opposite of obesity – both are associated with excess fat accumulation, and as a result, hold the same danger for patients who may contract COVID-19. Obesity presents with fat accumulated in the central area of the body, primarily in the abdomen, and is associated with diseases such as diabetes, high blood pressure, high cholesterol, and cardiovascular disease. However, lipedema presents with peripheral fat in the extremities, while the abdomen and/or waist are typically unaffected. But because both diseases increase a patient’s BMI, misdiagnoses are common and destructive. This illustrates one reason why BMI is not a biologically valid way to diagnose obesity or lipedema, but all the while makes women with Lipedema at high risk for becoming severely ill from COVID-19.
Take Every Precaution


COVID-19 vaccines (initial doses and boosters) and preventive measures for COVID-19 are important, especially if you are older, have multiple or severe health conditions, and/or carry excess fat on your body, such as individuals with Lipedema are known to suffer from. Learn more about CDC’s COVID-19 vaccination recommendations, including how medical conditions and other factors inform recommendations. If you have a medical condition, learn more about Actions You Can Take.
Questions about Lipedema?
Even with all the challenges presented by lipedema, there are those who you can trust. Dr. Wright continues to strive for better education, research, and coverage for the lipedema community. Do not let these challenges bring you down even further; let Dr. Wright and his expert team help you to reduce the symptoms of lipedema and live your life. Dr. Wright can help find the right procedure to help manage your lipedema symptoms, such as lymphatic drainage massage. Don’t let lipedema take over your life; contact us today!
Kompaniyets L, Goodman AB, Belay B, et al. Body Mass Index and Risk for COVID-19–Related Hospitalization, Intensive Care Unit Admission, Invasive Mechanical Ventilation, and Death — United States, March–December 2020. (2021). MMWR Morb Mortal Wkly Rep 2021;70:355–361.
O’Hearn M, Liu J, Cudhea F, Micha R, Mozaffarian D. (2021). Coronavirus Disease 2019 Hospitalizations Attributable to Cardiometabolic Conditions in the United States: A Comparative Risk Assessment Analysis. Journal of the American Heart Association. 2021 Feb;10(5):e019259.




